Mosquito-borne Diseases
Background
The United States was once home to mosquito-borne diseases that caused many fatalities, including yellow fever and malaria, both of which were eliminated in the U.S. during the 20th century. Public health programs, socioeconomic changes, and modern conveniences such as indoor plumbing and widespread use of window screens and air conditioning have served to reduce the burden of mosquito-borne diseases in the U.S.
However, the introduction of West Nile Virus (WNV) to North America in 1999 and an increase in the affordability and availability of international travel have since changed the landscape of mosquito-borne diseases in the U.S. WNV is now endemic, or'native' to every state except Alaska and Hawaii, resulting in thousands of infections, some of these fatal, every year.
Mosquito-borne Disease Transmission
There are more than 3,500 species of mosquito around the world, but only a very small number of these transmit diseases.
Mosquitoes are active in temperatures between 50 and 95▫F, and thrive at temperatures near 80▫F. They require freshwater sources to complete their life cycle. Pregnant females lay their eggs in standing water (lakes, ponds, swamps, and manmade sources). The eggs may hatch and become adult mosquitoes within two weeks but can also remain viable in water for several months (overwinter) and hatch in the spring. In addition, mosquito populations will often increase dramatically after catastrophic events such as hurricanes and floods due to accumulation of standing water that serve as breeding sites.
Feeding
Females of some mosquito species feed on blood to aid in egg production. Disease transmission occurs when the mosquitoes bite a human or animal that is carrying the disease and then feeds on another human or animal.
Mosquito bites typically appear as red bumps that may become itchy. Most often treatment of the bite requires minimal first aid, but severe allergic reactions can occur.
Hosts
Mosquito-borne diseases can be divided into two types, those for which humans are the primary host in the transmission cycle and those that are zoonotic, meaning passed between humans and animals, and require another animal host for transmission. Primary hosts and disease transmission cycles are shown in (Figure 1).
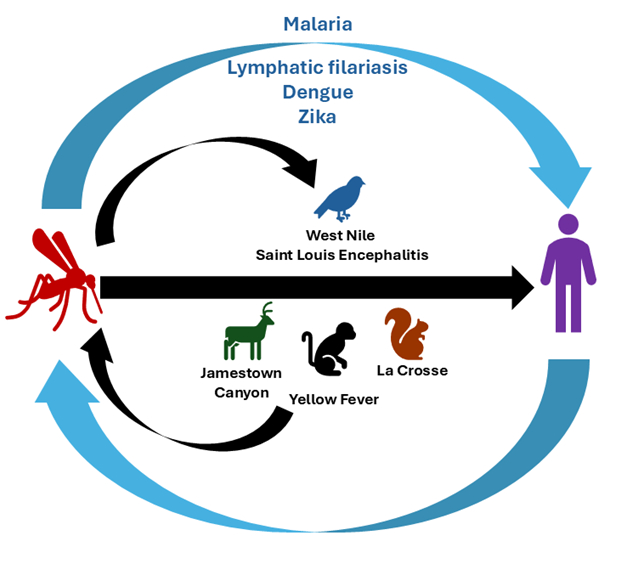
Figure 1. Human and zoonotic mosquitos-borne diseases. Humans are the primary hosts for some mosquito-borne diseases (blue arrows and text), while animals are the primary hosts of others (black arrows and text) and humans are a dead-end host, meaning that they are not able to transmit the infection.
*Yellow fever can be spread from humans to mosquitos in Sub-Saharan Africa, but not in the Americas.
Mosquitoes and the Diseases they Spread
Mosquitoes that carry diseases affecting humans belong to the Culicidae genetic family and are predominantly species of Culex, Aedes, and Anopheles classification (Figure 2). All of these species live in tropic and subtropic regions on all continents except Antarctica. In addition, both Culex and Anopheles mosquitoes live in temperate regions.
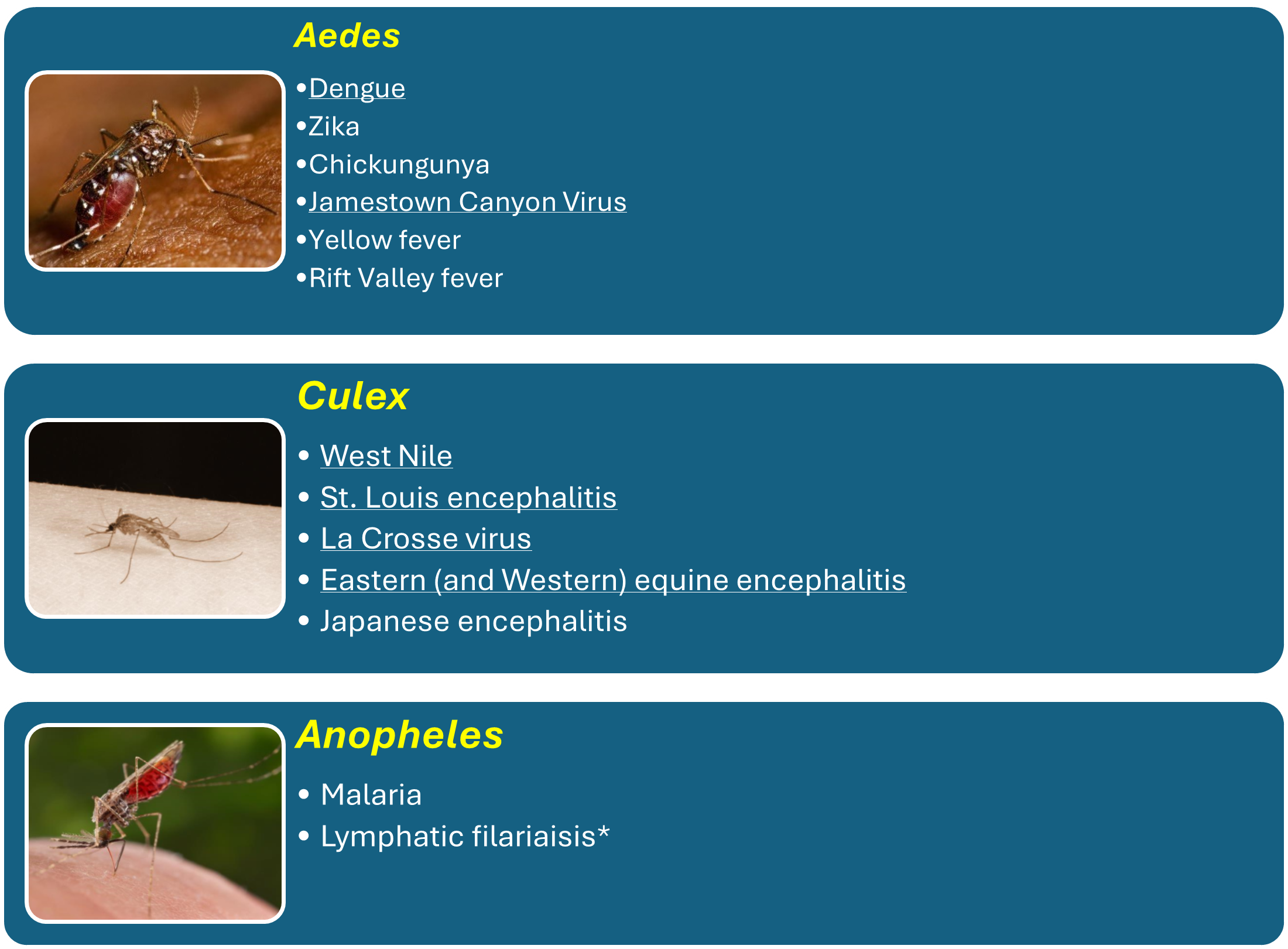
Images from PHIL, CDC. Sources: Department of Molecular Virology and Microbiology, Baylor College of Medicine and Mosquito Fact Sheet, European Centre for Disease Control and Prevention
Figure 2. Mosquitos and the diseases they spread. Aedes, Culex, and Anopheles mosquitoes and some of the diseases they carry that affect humans. Those underlined are endemic, or native, to the United States. Mosquitos and the diseases they spread: Mosquito - Aedes: Diseases spread by Aedes: Dengue (native to the United States) Zika Chikungunya Jamestown Canyon Virus (native to the United States) Yellow fever Rift Valley fever | Mosquito - Culex: Diseases spread by Culex: West Nile (native to the United States) St. Louis encephalitis (native to the United States) La Crosse virus (native to the United States) Eastern (and Western) equine encephalitis (native to the United States) Japanese encephalitis | Mosquito - Anopheles: Diseases spread by Anopheles: Malaria Lymphatic filariaisis* (Lymphatic filariasis can also be carried by species of Aedes, Culex, Mansonia, and Coquillettidia, depending on geographic location and setting.)
* Lymphatic filariasis can also be carried by species of Aedes, Culex, Mansonia, and Coquillettidia, depending on geographic location and setting.
Mosquito-borne Diseases of the United States
All mosquito-borne diseases are bloodborne because they are passed from one host's blood to another, indirectly by mosquitoes. Although rare, there have been instances of direct blood-to-blood transmission of mosquito-borne diseases through needlesticks, blood transfusions, and organ transplants.
West Nile Virus Disease
The most common mosquito-borne disease in the U.S. is West Nile Virus (WNV), which is present in all 48 contiguous states, as well as the District of Columbia, and Puerto Rico. It is the most geographically widespread mosquito-borne virus in the world due to globalization, and its introduction and spread to the United States began in New York in1999. Since then, it quickly spread throughout the nation.
WNV may be asymptomatic in about 80% of people, but symptoms that may occur include:
- Headache
- Fatigue
- Sore joints and muscles
- Upset stomach and/or diarrhea
- Rash with flat discolored spots and raised red bumps (maculopapular)
Less than 1% of people have neurological symptoms, all of which are a medical emergency. These include:
- Meningitis – infection and swelling of the membranes around the spinal cord.
- Symptoms include severe headache, fever, and stiff neck. Other possible symptoms are weakness, confusion, lack of appetite, nausea, light sensitivity, seizures.
- Encephalitis – infection and swelling of the brain.
- Symptoms include headache, fever, weakness, and fatigue. Other possible symptoms are stiff neck, hallucinations, seizures, loss of feeling in body parts, irregular movements, trouble with speech or hearing, loss of consciousness or coma.
- Acute flaccid myelitis – infection of spinal cord gray matter that is the central “hub” for nerve signals in and out of the brain.
- Symptoms include sudden weakness, loss of muscle tone, or loss of reflexes in arms or legs. Other possible symptoms are facial droop or weakness, difficulty moving eyes, trouble swallowing, slurred speech, pain in arms or legs.
People cannot transmit WNV back to mosquitoes but there have been instances of direct transfer to other people via blood transfusion and organ donation. In addition, mothers can transmit WNV to their infants during pregnancy, childbirth, and by breast feeding but the risk of transmission of WNV via these routes is very low.
Quick Facts: Mosquito-borne Diseases in the U.S., 2024
In 2024, there were over 7,500 reported cases of locally acquired mosquito-borne disease in the United States and its territories.
Since its introduction to the U.S., West Nile Virus (WNV) has resulted in roughly 60,000 reported cases of disease, 28,000 hospitalizations, and nearly 3,000 deaths.
In fact, WNV is usually the most commonly acquired mosquito-borne infection in the U.S. But in 2024, there was a widespread outbreak of Dengue Virus in the Americas and Caribbean, resulting in the highest number of locally-acquired infections from a single mosquito-borne illness (6,542) ever recorded in a year in the U.S.
Dengue was spread from mosquitoes to humans in three of the 48 contiguous states including California (18 cases), Florida (85) and Texas (2). Most infections (6,228) were acquired in Puerto Rico and 209 were acquired in the U.S. Virgin Islands.
Other locally acquired, mosquito-borne infections in the U.S. in 2024 were:
- West Nile Virus (1,466 cases)
- La Crosse Encephalitis Virus (35 cases)
- Easter Equine Encephalitis (19 cases)
- St. Louis Encephalitis (1)
- Jamestown Canyon Virus (21)
Dengue fever
Humans are the primary host for Dengue virus (DENV), and dengue fever has a long history. The first suspected dengue-like epidemic was reported in 1635 in the West Indies. Dengue spread rapidly to urban ports around the world, including the United States, in the 18th and 19th centuries as the global shipping industry expanded. Today, DENV is commonly found in Aedes mosquitoes in tropical and semitropical regions of the Americas, which includes islands in the Caribbean (including Puerto Rico) and Pacific, Mexico, Central America, and all but southern tip of South America.
In the United States, most instances of DENV infection are associated with international travel, but during outbreaks, local transmission in the contiguous 48 states has occurred. Between 2010 and 2024, local DENV transmission was recorded in California (20 cases), Texas (42 cases) and Florida (534 cases).
Many symptoms of dengue fever are distinct from the endemic zoonotic viruses. The most common symptom is a high fever (often up to104▫F) that lasts 24-48 hours, with any of the following:
- Head and body (muscle, joint and bone) aches and pains
- Nausea, vomiting
- Rash
The head and body aches described can be severe, so illnesses caused by DENV is sometimes referred to as 'break-bone fever'. About 1 in 20 (5%) of people with symptomatic dengue fever suffer severe symptoms. DENV can cause Dengue Hemorrhagic Fever, a severe form of the disease that causes internal bleeding, which is a medical emergency. Symptoms of severe disease are life-threatening and usually begin 24-48 hours after the fever has gone away. These include:
- Abdominal pain or tenderness
- Bleeding from the nose or gums
- Frequent vomiting (especially blood)
- Blood in stools
- Feeling very tired or restless
People who have had dengue before, those with weakened immune systems, pregnant women, and children under the age of five are at higher risk of developing severe dengue.
Eastern Equine Encephalitis
Like WNV, Eastern Equine Encephalitis (EEE) is a zoonotic disease for which birds are the primary host. Most people who are infected remain asymptomatic. When symptoms of EEE do develop, they are very similar to those of WNV. Most cases of EEE have occurred in states east of the Mississippi River.
Reports of EEE infections are rare in the U.S., averaging less than 10 illnesses per year since 2003, but nearly all reported infections result in serious illness. For instance, in 2024, 19 cases were reported and all of these involved neurological disease (see Quick Facts Box). About 30% of people who develop EEE neurological disease die, and many of those that survive have long-term problems. Note that Western Equine Encephalitis occurs in the western U.S. but no cases have been recorded since the 1990s.
St. Louis Encephalitis
Like other zoonotic mosquito-borne diseases, St. Louis Encephalitis is usually asymptomatic, and when symptoms develop, they are very similar to WNV and EEE. Although still very rare, there were an average of 14 cases per year between 2003 and 2024. Of these, roughly 68% were hospitalized and less than 7% of patients died. Most St. Louis Encephalitis Infections occurred in the South Central and Western parts of the United States.
La Crosse Virus
Unlike WNV, EEE, and St. Louis Encephalitis, the primary hosts for La Crosse are squirrels and other small rodents. La Crosse is like other zoonotic mosquito-borne viruses native to the U.S. in that virus infections may be asymptomatic or cause serious symptoms such as encephalitis. La Crosse is unique however, because nearly all of those who become symptomatic are children, the majority of whom develop neuroinvasive disease and require hospitalization.
Jamestown Canyon Virus
A similar mosquito-borne disease is Jamestown Canyon Virus. Jamestown Canyon Virus is a member of the same viral family as La Crosse and is native to the U.S. It is transmitted from several mosquito types, and its primary hosts are deer and other wild, hooved mammals (elk, moose, mountain goats, etc.). Most human cases occur in the upper Midwest and symptoms are similar to those of La Crosse, with neuroinvasive disease and encephalitis as possible outcomes. About half of patients with Jamestown Canyon Virus are hospitalized.
Travel-related Mosquito-borne diseases
Malaria
Malaria is the deadliest of the mosquito-borne diseases. The World Health Organization estimates that in 2023, about 263 million people from 83 countries acquired malaria and of those, 597,000 died. About 2,000 cases occur in the U.S. each year, but these are nearly all travel-related.
Malaria is caused by the parasite Plasmodium spp. carried by the Anopheles mosquito. When the mosquito bites a person, the parasites enter the bloodstream and invade the liver, undergoing life cycle changes, and then are released into the bloodstream where they invade red blood cells. In the blood cells, Plasmodium parasites mature and grow larger, rupturing, or bursting, the red blood cells, causing symptoms. In this blood stage, the parasites can infect another biting mosquito.
Malaria is characterized by symptoms of fever, headache, and chills that occur in cycles, or “attacks.” These attacks correspond with the parasite maturation during the blood stage and usually start with shivering and chills, followed by fever and then recovery. Other common symptoms may include headache, nausea and vomiting, diarrhea, and muscle or joint pain.
Malaria can quickly become severe and sometimes fatal. Malaria caused by P. falciparum can lead to cerebral malaria, where infected red blood cells obstruct flow of blood in the brain, causing seizures, confusion, and brain damage. Other serious complications of malaria that can lead to death include acute renal failure and acute respiratory distress syndrome. Prescription medications that prevent travel-related malaria are available and should be considered when visiting or working in areas where malaria is endemic.
Yellow Fever
Yellow fever virus (YFV) is transmitted primarily by the Aedes spp. mosquito and is no longer endemic to the U.S. In forested and jungle areas of central and northern South America, Trinidad and Tobago, and Panama, monkeys and other non-human primates are required hosts for YFV and the disease cannot be spread directly from mosquitoes to humans (Figure 1). In forested Sub-Saharan Africa, however, yellow fever is transmitted this way but can also be spread from human to mosquito to human in urban areas.
Like malaria, outbreaks of yellow fever occurred in the United States over the centuries, with the last know epidemic occurring in New Orleans in 1905. Outside of the U.S., where yellow fever is endemic, small epidemics occur with some regularity. For example, in 2023, there were over 430 cases of yellow fever in Africa, with Sierra Leone (160) and South Sudan (104) having the greatest number of illnesses. However, most countries affected had fewer than 10 cases.
Common symptoms of yellow fever include fever, headache, muscle pain with severe backache, loss of appetite, and nausea or vomiting. While most people recover within 4 days, about 15% of people develop toxic, systemic disease leading to the recurrence of fever and hemorrhaging in organ systems, especially the liver and kidneys, resulting in jaundice, abdominal pain, and vomiting. Up to 50% of patients who develop the more toxic form of yellow fever die.
Note that a vaccine against yellow fever is available and often required prior to travel in endemic countries
Chikungunya
Chikungunya is caused by a virus that is unrelated to WNV, DENV and YFV. It can be found on all continents except Australia and Antarctica. It is spread primarily by Aedes spp. mosquitoes and causes symptoms like those of DENV including fever and severe, sometimes debilitating joint pain. Joint swelling, muscle pain, headache, fatigue, nausea, and rash may also occur. Unlike Dengue, Chikungunya is not a hemorrhagic fever (one that causes internal bleeding) and very few die from their illness. One rare complication associated with Chikungunya is Guillain-Barré syndrome, a condition caused by autoimmune attack of nerve tissue, resulting in muscle weakness and sometimes paralysis. If there is an outbreak of Chikungunya ongoing in your destination country, a vaccine may be available from your healthcare provider.
Note that Chikungunya is considered a travel-associated mosquito-borne infection, but local transmission occurred in Puerto Rico and other US territories as well as Florida (2014) and Texas (2015). No local transmission of Chikungunya has been reported in the U.S. or its territories since 2019.
Zika Virus
Zika virus (ZIKV), spread by the Aedes spp. of mosquito, is in the same family of viruses (Flaviviridae) as WNV and DENV. A unique feature of ZIKV is that it can be sexually transmitted from a host carrier (infected with ZIKV) to a healthy partner. Further, ZIKV can cause severe birth defects.
Zika virus (ZIKV) was originally isolated from a monkey in a Ugandan forest during a scientific study of yellow fever in 1947. Since that time, ZIKV spread exclusively within Africa until 2007, when it appeared in Micronesia, a Pacific Island. By 2014, ZIKV had reached the Americas, causing an epidemic in Brazil that began in 2015 and spread throughout South and Central America as well as the Caribbean. Widespread transmission also occurred in the U.S. Virgin Islands and Puerto Rico. While there were limited cases in the contiguous U.S. between 2016 and 2017 (Texas: 92 cases, Florida: 143 cases), no Zika transmission has been reported in the U.S. or its territories since 2019.
Many people who acquire Zika are asymptomatic. When symptoms occur, they mirror those of Dengue fever and Chikungunya. Unlike Dengue, Zika is not a hemorrhagic fever. Very few adults die from Zika, but infection may lead to Guillain-Barré syndrome in rare cases. In addition, ZIKV does have a unique transmission pathway that may result in serious complications for women who are pregnant who can pass the infection to their fetus.
ZIKV is known to be transmitted through blood and body fluids. Zika has been found in blood, saliva, urine, vaginal secretions, semen, and breast milk. Because of this, ZIKV has the unique classification as a mosquito-borne, sexually transmitted disease. There is evidence that ZIKV can be passed between partners during sexual encounters. When a woman who is pregnant acquires Zika through a sexual partner or through a mosquito bite, ZIKV can pass through the placenta, infecting the fetus, which may cause birth defects. This is known as Congenital Zika Syndrome.
Congenital Zika Syndrome can result in birth defects of the brain or eye or cause a pattern of developmental problems that may manifest later in life. After passing through the placenta, the ZIKV infects neural (brain and nerve) tissue causing inflammation and damage. Possible outcomes of Congenital Zika Syndrome include, but are not limited to:
- Microencephaly (smaller than average brain size)
- Seizures
- Vision problems and hearing loss
- Difficulty feeding and swallowing
- Contractures (permanent shortening of muscle fibers causing stiff muscles and reduced movement of joints)
Lymphatic Filariasis
Like malaria, Lymphatic filariasis is a parasitic disease spread to humans by mosquitoes. It has been eliminated in many tropical and sub-tropical areas where it was once endemic but there is ongoing transmission in all of Sub-Saharan Africa, India, Nepal, Myanmar, Malaysia, Indonesia, Philippines, Papua New Guinea, New Caledonia, Fiji, and Haiti.
Also known as elephantiasis, the disease occurs when parasitic larvae transmitted by mosquitoes develop into adult worms in the lymphatic system (or lymph nodes) producing offspring called microfilariae. These microfilariae migrate into the bloodstream to be ingested by mosquitoes during a blood meal, thus completing the life cycle.
Symptoms of infection include thickening of the skin and underlying tissue, inflammation in the lymph nodes (elephantiasis). Areas most often affected include the arms, legs, breasts, vulva, scrotum and testicles. Chronic infections can be extremely painful and disfiguring. According to the World Health Organization (WHO), an estimated 36 million across the globe live with chronic and disfiguring lymphatic filariasis.
Other Mosquito-borne Diseases of Concern to Overseas Workers
Although OSHA's authority is limited to employment performed within geographical boundaries of the United States and its territories, this information should serve as a resource for employers to keep employees safe.
The following list of mosquito-borne diseases is not comprehensive, but provides links to information about other, rarer, mosquito-borne diseases that can be acquired overseas.
- In the Caribbean and tropical regions of Central and South America, mosquitoes may carry Oropouche although biting midges are the primary vector.
- In Australia and parts of Oceana, mosquito-borne diseases include Kunjin virus, Ross River and Barmah Forest viruses as well as Murray Valley Encephalitis.
- In tropical and subtropical Asia, Japanese encephalitis can be found, whereas Rift Valley Fever is widespread in Africa.
Workers should check the CDC's Travelers' Health destination pages to learn about steps to stay healthy while living and working in your destination.

