Hospitals eTool
Administration » Admissions and Records
Hospital department responsible for the flow of patients and the processing of admissions, discharges, transfers, and also most procedures to be carried out in the event of a patient's death. [See OSHA’s statement regarding its choice of focus points for this hospital area]
Typically, the first encounter of patients being admitted to the hospital is with the admitting staff. Patients may harbor organisms that cause seasonal and pandemic influenza; norovirus; Ebola; Middle East Respiratory Syndrome (MERS), tuberculosis, methicillin-resistant Staphylococcus aureus (MRSA), other potentially drug-resistant organisms, among other infectious diseases.
Infectious diseases are caused by agents that are transmissible through one or more different routes, including the contact, droplet, airborne, and bloodborne routes. The transmission of infectious agents through the bloodborne route—a specific subset of contact transmission—is defined in the Bloodborne Pathogens (BBP) standard, 29 CFR 1910.1030 (See the Bloodborne Pathogens section below). Employees who work in admitting areas are likely to be exposed to infectious diseases by the airborne, droplet and contact routes.
An effective infection control program normally relies upon a multi-layered and overlapping strategy of engineering, administrative and work practice controls, and PPE. It is OSHA’s intent in this eTool to highlight some – not all – of the controls that would be necessary to the development and implementation of an effective program. Implementing the controls highlighted here alone will not typically protect workers from infection hazards.
Follow standard and transmission-based precautions to prevent worker infections (see also the OSHA page: Worker protections against occupational exposure to infectious diseases). Early identification and isolation of sources of infectious agents (including sick patients), proper hand hygiene, worker training, effective engineering and administrative controls, safer work practices, and appropriate personal protective equipment (PPE), among other controls, help reduce the risk of transmission of infectious agents to workers.
Employers must comply with the PPE Standard, 29 CFR 1910 Subpart I, and the OSH Act’s General Duty Clause, 29 U.S.C. 654(a)(1), to protect their workers from infectious disease hazards. The General Duty Clause requires each employer to “furnish to each of his employees employment and a place of employment which are free from recognized hazards that are causing or are likely to cause death or serious physical harm to his employees.” Employers must also comply with the BBP standard to the extent that there is “occupational exposure” (i.e., to the extent employers should reasonably anticipate contact with blood or other potentially infectious materials (OPIM) that may result from the performance of duties).
OSHA provides agent-specific guidance for a variety of pathogens that workers in hospital settings may encounter. See OSHA's Safety and Health Topics Pages for Biological Agents and Bloodborne Pathogens and Needlestick Prevention for additional information.
In this module, OSHA provides additional guidance specifically for:
- Tuberculosis
-
Hazard
Exposure of staff to Tuberculosis (TB) from patients coughing, speaking, sneezing, etc. during admissions.
TB is caused by a bacterium called Mycobacterium tuberculosis and is spread by airborne droplets generated when a person with TB disease coughs, speaks, sneezes, etc. Infection occurs when a susceptible person inhales droplet nuclei containing the bacteria, which then become established in the body.
TB transmission has been documented in healthcare settings where healthcare workers and patients come in contact with people who have TB disease (see CDC Burden of TB in the United States page). An additional hazard is present because of multidrug-resistant (MDR) TB. MDR organisms are resistant to the drugs that are normally used to treat TB, such as the antibiotics Isoniazid and Rifampin (see CDC Drug-Resistant TB page).
Admissions departments can request of any patient who is coughing that they don a disposable surgical mask immediately upon approaching the admissions desk to help reduce employees’ exposure to TB.
Requirements under OSHA's Respiratory Protection Standard, 29 CFR 1910.134
Employers must comply with applicable provisions of OSHA’s Respiratory Protection standard, 29 CFR 1910.134, for using respirators to protect against TB hazards.
Recognized Controls and Work Practices
The CDC discusses three types of controls for TB infection in healthcare settings:
- Administrative controls to minimize the number of areas where exposure to TB can occur
- Environmental controls to reduce the concentration of TB
- The use of respiratory protection in situations that pose a high risk for exposure
Recognized controls and work practices include:
- Providing an area in the Admissions area that is ventilated separately for TB patients (i.e., patients with suspected or confirmed TB) in facilities in which TB patients are frequently treated. If this is not possible, ensuring that TB patients wear surgical masks, and stay in the Admissions area the minimum amount of time possible, and be transferred promptly to isolation rooms.
- Healthcare facilities serving populations that have a high prevalence of TB may need to supplement the general ventilation or use additional engineering controls in general-use areas where TB patients are likely to go (e.g., waiting-room areas, emergency departments, and radiology suites). These engineering controls include:
- A single-pass, non-recirculating system that exhausts air directly to the outside.
- A recirculation system that passes air through HEPA (High Efficiency Particulate Air) filters before re-circulating it to the general ventilation system.
Additional Information
- Enforcement Procedures and Scheduling for Occupational Exposure to Tuberculosis. OSHA Directive CPL 02-02-078, (June 30, 2015). Contains information concerning OSHA’s general enforcement policy and procedures for conducting inspections and issuing citations related to occupational tuberculosis (TB) hazards.
- Inspection Guidance for Inpatient Healthcare Settings. (June 25, 2015). OSHA memorandum establishing guidance for inspections conducted in inpatient healthcare settings.
- Fit Testing Requirements for Employees Who Wear Respirators to Protect against M. Tuberculosis, SARS, Smallpox, and Monkeypox. (February 5, 2004).
- Tuberculosis. OSHA Safety and Health Topics Page.
- Tuberculosis. Centers for Disease Control and Prevention.
- Lewinsohn, D.M., et al. Official American Thoracic Society/Infectious Diseases Society of America/Centers for Disease Control and Prevention Clinical Practice Guidelines: Diagnosis of Tuberculosis in Adults and Children." Clinical Infectious Diseases, Vol 64, Issue 2, 2017: e1-e33.
- Respiratory Protection Program Training and Resources. American Association of Occupational Health Nurses (AAOHN). This online training program prepares hospital staff for respiratory protection in the workplace.
- Also see Hospital-wide Hazards – Tuberculosis.
- Influenza (Flu)
-
Hazard
Exposure of staff to infectious diseases, such as seasonal or pandemic influenza*.
Healthcare workers, particularly physicians and nurses, are at a higher risk of acquiring influenza than healthy adults working in non-healthcare settings (Kuster et al., 2011).
Influenza can be transmitted by both symptomatic and asymptomatic individuals through respiratory tract secretions, mucus, cough and sneeze aerosols, and contaminated hands and materials.
Recognized Controls and Work Practices
- Encourage workers to get vaccinated and make vaccinations available to workers. The Centers for Disease Control and Prevention (CDC), the Advisory Committee on Immunization Practices (ACIP), and the Healthcare Infection Control Practices Advisory Committee (HICPAC) recommend that all U.S. healthcare workers get vaccinated annually against influenza.
- Modify patient intake, triage, and other service areas to increase space between workers, coworkers, and patients and provide barriers against transmission when applicable (e.g., install sneeze guards or partitions).
- Isolate and group flu patients when possible.
- Limit patient transport. Conduct exams and procedures at the bedside, instead of transporting the patient to other areas of the facility. Place a surgical mask on the patient, if possible, when they are being transported.
- Restrict visits for patients in isolation.
- Use proper respiratory and cough etiquette and encourage hand washing by patients and visitors.
- Wash hands with soap and water for at least 20 seconds before and after contact with patients, after using PPE, and after touching contaminated surfaces; use an alcohol-based hand rub if soap and water are not available.
- When using soap and water, rub soapy hands together for at least 20 seconds, rinse hands with water, and dry completely.
- If soap and water are not available, use of an alcohol-based hand rub is helpful as an interim measure until hand washing is possible. When using an alcohol-based hand rub, apply liquid to palm of hand, cover all surfaces of the hands with the liquid, and rub hands together until dry.
- Monitor yourself for symptoms of the flu, such as fever or feeling feverish/chills, cough, sore throat, runny or stuffy nose, muscle or body aches, headaches, and fatigue (tiredness).
- Follow standard cleaning and disinfection methods.
* While the recognized control and work practices that protect workers from exposure to seasonal and pandemic influenza are basically the same, consult the CDC’s “Interim Guidance for Infection Control Within Healthcare Settings When Caring for Confirmed Cases, Probable Cases, and Cases Under Investigation for Infection with Novel Influenza A Viruses Associated with Severe Disease,” in the event of an influenza pandemic to determine if any higher level precautions should be implemented (i.e., the use of respirators rather than surgical masks when HCWs are engaged in direct patient care).
Additional Information
While the recognized control and work practices that protect workers from exposure to seasonal and pandemic influenza are basically the same, consult the CDC’s “Interim Guidance for Infection Control Within Healthcare Settings When Caring for Confirmed Cases, Probable Cases, and Cases Under Investigation for Infection with Novel Influenza A Viruses Associated with Severe Disease,” in the event of an influenza pandemic to determine if any higher level precautions should be implemented (i.e., the use of respirators rather than surgical masks when HCWs are engaged in direct patient care).
- Kuster, P. et al. (2011) Incidence of Influenza in Healthy Adults and Healthcare Workers: A Systematic Review and Meta-Analysis. PLoS ONE, 6(10).
- Seasonal Flu
- Seasonal Flu. OSHA Safety and Health Topics Page.
- Prevention Strategies for Seasonal Influenza in Healthcare Settings. Centers for Disease Control and Prevention.
- Seasonal Influenza Vaccination – Important Protection for Healthcare Workers. OSHA Fact Sheet.
- Influenza Vaccination Information for Health Care Workers. Centers for Disease Control and Prevention.
- Pandemic Influenza
- Pandemic Influenza. OSHA Safety and Health Topics Page.
- How to Protect Yourself in the Workplace during a Pandemic. OSHA QuickCardTM.
- What Employers Can Do to Protect Workers from Pandemic Influenza. OSHA Fact Sheet.
- Also see Hospital-wide Hazards – Influenza.
- Multidrug-Resistant Organisms
-
Hazard
Exposure of staff and patients to Multidrug Resistant Organisms (MDROs) resulting in nosocomial (hospital-acquired) infections.
Common examples of these organisms include:
- Carbapenem-resistant Enterobacteriaceae(CRE) are a family of germs that can become carbapenem-resistant, including Klebsiella pneumoniae and Escherichia coli (E. coli).
- Clostridium difficile (C. Diff). Clostridium difficile is a spore-forming, Gram-positive anaerobic bacillus. It is a common cause of antibiotic-associated diarrhea
- Extended-spectrum beta-lactamases (ESBLs). ESBLs of concern are resistant to cephalosporins and monobactams.
- Methicillin/Oxacillin-resistant Staphylococcus aureus (MRSA), which includes Vancomycin-intermediate Staphylococcus aureus (VISA) and Vancomycin-resistant Staphylococcus aureus (VRSA) is addressed below and also in Hospital Wide Hazards – MRSA.
- Multidrug-resistant Acinetobacter baumannii (MDR-Ab) is a gram-negative bacterium that can colonize the skin of infected patients.
- Multi-drug-resistant Tuberculosis (MDR-TB) is addressed in Hospital-Wide Hazards – Tuberculosis.
- Penicillin-resistant Streptococcus pneumoniae (PRSP). Pneumococcal disease is an infection caused by Streptococcus pneumoniaebacteria, sometimes referred to as pneumococcus. Pneumococcus can cause many types of illnesses, including ear infections and meningitis.
- Vancomycin-resistant enterococci (VRE). Enterococci are bacteria that can live in the human intestines and female genital tract without causing disease or infection (often called colonization). However, enterococci can cause infections of the urinary tract, the bloodstream, or of wounds associated with catheters or surgical procedures. Vancomycin is usually the drug of choice for treating these bacteria. However, VRE are resistant to Vancomycin.
The CDC provides guidelines and recommends controls for MDRO hazards.
Additional Information
- Management of Multidrug-Resistant Organisms in Healthcare Settings. Centers for Disease Control and Prevention (CDC).
- Healthcare: Infectious Disease. OSHA Safety and Health Topics Page.
- Healthcare-associated Infections (HAI). Centers for Disease Control and Prevention (CDC).
- Antibiotic / Antimicrobial Resistance. Centers for Disease Control and Prevention (CDC).
- Understanding Antimicrobial (Drug) Resistance. National Institute of Allergy and Infectious Diseases (NIAID).
- Also see Hospital-wide Hazards - MDRO - Multidrug-Resistant Organisms and Infection.
Methicillin-Resistant Staphylococcus aureus (MRSA includes VRSA and VISA)
Hazard
Admissions staff can be exposed to MRSA through contact with infected individuals (e.g., patients, visitors or staff members) or individuals who may be colonized. Colonization means that the organism is present in or on the body but is not causing illness. Many patients who are admitted to the hospital may already be colonized. An employee who has been colonized can become a carrier and spread infection to other healthcare workers and patients.
Recognized Controls and Work Practices
Infection control is the key to preventing the spread of MRSA.
- Ensure the availability of adequate facilities and supplies that promote good hand hygiene.
- Perform routine housekeeping in the admissions area, including decontaminating equipment and surfaces with detergent-based cleaners. Use EPA-registered disinfectants and sterilants when appropriate.
For more information, see Hospital-wide Hazards - Methicillin-resistant Staphylococcus aureus (MRSA). Provides links with general information, answers specific questions for employers and employees, and offers resources for a variety of workplace settings and activities, including healthcare, schools, athletics, and childcare.
Also see Hospital-wide Hazards - MDRO - Multidrug-Resistant Organisms and Infection.
- Bloodborne Pathogens (BBP)
-
Bloodborne pathogens are pathogenic microorganisms present in human blood that can cause disease in humans. These pathogens include, but are not limited to, Hepatitis B Virus (HBV), Hepatitis C Virus (HCV), Human Immunodeficiency Virus (HIV) and Viral Hemorrhagic Fevers (e.g. Ebola). [29 CFR 1910.1030(b)]
Hazards
Occupational exposure to blood or other potentially infectious materials (OPIM) during admissions.
Requirements under OSHA's Bloodborne Pathogens Standard, 29 CFR 1910.1030
The Bloodborne Pathogens Standard requires precautions when there is occupational exposure to blood or OPIM (as defined by the standard). Under the standard, OPIM means (1) the following human body fluids: semen, vaginal secretions, cerebrospinal fluid, synovial fluid, pleural fluid, pericardial fluid, peritoneal fluid, amniotic fluid, saliva in dental procedures, any body fluid that is visibly contaminated with blood, and all body fluids in situations where it is difficult or impossible to differentiate between body fluids; (2) any unfixed tissue or organ (other than intact skin) from a human (living or dead); and (3) HIV-containing cell or tissue cultures, organ cultures, and HIV- or HBV-containing culture medium or other solutions; and blood, organs, or other tissues from experimental animals infected with HIV or HBV.
OSHA requires employers to ensure that the biosafety officer or other responsible person conducts an exposure determination to determine the exposure of workers to blood or OPIM throughout the hospital setting. [29 CFR 1910.1030(c)(2)(i)].
For more information, see Hospital-wide Hazards - Bloodborne Pathogens.
Hazard
The admissions and records staff is exposed to ergonomics-related risk factors, such as repetitive movements, forceful exertions, excessive reaching above shoulder-height while filing, and awkward posture during file management. Exposure to ergonomic hazards may lead to musculoskeletal disorders (MSDs) including carpel tunnel syndrome, tendonitis, or tenosynovitis.
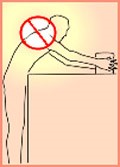
Reaching/Lifting: Frequent reaching above the shoulders or elevated extended reaches for files can cause back and shoulder injury.
- Repeatedly lifting the arms or repeatedly reaching can irritate the tendons or bursa of the shoulder leading to bursitis or rotator cuff tendonitis. Supporting or lifting a load with the arm elevated or extended can lead to injuries such as muscle strain or rotator cuff tears.
- Working with the arms in an elevated posture or behind the back can lead to impingement injuries such as thoracic outlet syndrome.
Recognized Controls and Work Practices
- Redesign or lower filing cabinets so they can be reached while maintaining the elbows in close to the body (neutral body posture).
- Use powered filing cabinets that move to any height.
- Use ladders or stools to access high files rather than reaching overhead.
- Avoid awkward postures (e.g., reposition work in front of worker rather than reaching above or behind to get files).
- Use proper lifting techniques:
- Avoid lifting/reaching or working above shoulder height.
- Avoid awkward postures, such as twisting while lifting.
- Lift items close to the body.
- Limit the weight of the item to be lifted.
Additional Information
- Musculoskeletal Disorders and Workplace Factors - A Critical Review of Epidemiologic Evidence for Work-related Musculoskeletal Disorders of the Neck, Upper Extremity, and Low Back. U.S. Department of Health and Human Services (DHHS), National Institute for Occupational Safety and Health (NIOSH) Publication No. 97-141, (July 1997).
- Hospital-wide Hazards – Work-related Musculoskeletal Disorders.
- Ergonomic Guidelines for Manual Material Handling. U.S. Department of Health and Human Services (DHHS), National Institute for Occupational Safety and Health (NIOSH) Publication No. 2007-131, (April 2007).
- Ergonomics. OSHA Safety and Health Topics Page.
- Inspection Guidance for Inpatient Healthcare Settings. (June 25, 2015). OSHA memorandum establishing guidance for inspections conducted in inpatient healthcare settings.
Hazard
Employees who use a computer intensively (e.g., admissions staff, data entry clerk), may develop work-related musculoskeletal disorders (MSDs) of the hand/arm, shoulder, neck, or back.
Recognized Controls and Work Practices
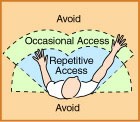


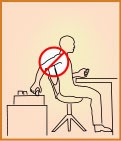
Look at the workstation layout and:
- Arrange materials and supplies in front of the body so they can be easily reached with the elbows in close to the torso.
- Provide adjustable, supportive padded chairs that support the forearms, legs, and low back. Arm rests allow the elbows to hang normally at the side of the body.
- Adjust work surface height so that there is sufficient room for the legs.
- Arrange monitor so that the most commonly viewed area is slightly below (about 20 degrees), horizontal eye level and can be seen without looking up, or leaning forward.
- Provide engineering controls to limit awkward positions (e.g., provide headsets for employees to use when answering phones).
- Use an adjustable keyboard tray that includes an adjustable mouse support that can be easily reached from a keying position. Employees need to keep wrists straight while typing and use wrist pads to rest on when not typing.
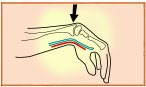
Repetitive Motions during hand-intensive tasks: Performing hand-intensive tasks (such as data entry, word processing) with a bent wrist creates considerable stress on the tendons and their sheaths as they are bent across the harder bones and ligaments that make up the outside structure of the wrist.
- As the fingers are activated, the tendon slides through the sheath and over the hard parts of the bent wrist, pinching the sheath between the tendon and these hard entities.
- Repetitive finger activations in these postures can create wear and tear on the tendon and the sheath.
- Prolonged forceful finger exertions in these postures can stretch and fray the tendon and create contact trauma to the sheath.
This wear and tear, fraying, or contact trauma can create irritation and swelling that may lead to tendonitis, tenosynovitis, and potentially carpal tunnel syndrome.
Additional Information
- For more information, see OSHA's Computer Workstations eTool, which can help identify, analyze and control musculoskeletal disorders in computer workstation tasks.
Hazard
An admissions area can become crowded with patients and families, many of whom are dealing with stressful situations and could become violent. Although anyone working in a hospital may become a victim of violence, staff who have direct contact with patients are at higher risk.
The effects of violence can range in intensity and include minor or serious physical injuries, temporary or permanent physical disability, psychological trauma, and even death.
The individual risk factors for violence vary from hospital to hospital depending on factors such as location, size, and type of care provided. Some common risk factors for hospital violence include the following:
- Working directly with patients or visitors who have a history of violence, abuse drugs or alcohol, and/or have access to firearms, knives, or other weapons;
- Working when understaffed;
- Long waits for service;
- Overcrowded, uncomfortable waiting rooms;
- Working alone;
- Poor environmental design;
- Inadequate security;
- Lack of staff training and policies for preventing and managing crises with potentially volatile patients;
- Unrestricted movement of the public; and
- Poorly lit corridors, rooms, parking lots, and other areas.
Recognized Controls and Work Practices
- Establishing a Workplace Violence Prevention program to address the risk of violent patients and that includes the following elements:
- Management Commitment to the Workplace Violence Prevention Program
- Employee Participation
- Worksite Analysis
- Hazard Prevention and Control
- Safety and Health Training
- Recordkeeping and Program Evaluation
- Implementing engineering controls, such as:
- Bolting down furniture
- Securing other items that could be used as weapons, such as phones, fire extinguishers, lamps, etc.
- Designing the waiting room to reduce tension from overcrowding.
- Installing and maintaining improved lighting and video surveillance.
- Training staff to recognize and de-escalate potentially violent situations and patients, to be alert for potential violence and suspicious behavior and report it, and to provide intervention measures including verbal, social, physical, and pharmacological interventions where feasible.
- Providing adequate staffing levels, with experienced clinicians on each shift.
- Providing adequate and well-trained security staff.
OSHA emphasizes that the controls discussed here do not represent the full array of controls that would comprise an effective Violence Prevention Program. For more information, please see Guidelines for Preventing Workplace Violence for Health Care & Social Service Workers. OSHA Publication 3148, (2016) and other documents referenced below.
Warning Signs of Increasing Anger/Violence include:
- Pacing and/or restlessness
- Clenched fists
- Increasingly loud speech
- Excessive insistence
- Threats
- Cursing
For additional information on Workplace Violence Prevention Program see Hospital-wide Hazards - Workplace Violence.
Additional Information
- Workplace Violence - Prevention Programs. OSHA Safety and Health Topics Page.
- Guidelines for Preventing Workplace Violence for Health Care & Social Service Workers. OSHA Publication 3148, (2016).
- Worker Safety in Hospitals: Caring for our Caregivers. OSHA.
- Enforcement Procedures and Scheduling for Occupational Exposure to Workplace Violence. OSHA Directive CPL 02-01-058 [CPL 02-01-052], (January 10, 2017).
- Inspection Guidance for Inpatient Healthcare Settings. (June 25, 2015). OSHA memorandum establishing guidance for inspections conducted in inpatient healthcare settings.
- Violence Occupational Hazards in Hospitals. U.S. Department of Health and Human Services (DHHS), National Institute for Occupational Safety and Health (NIOSH) Publication No. 2002-101, (April 2002).

