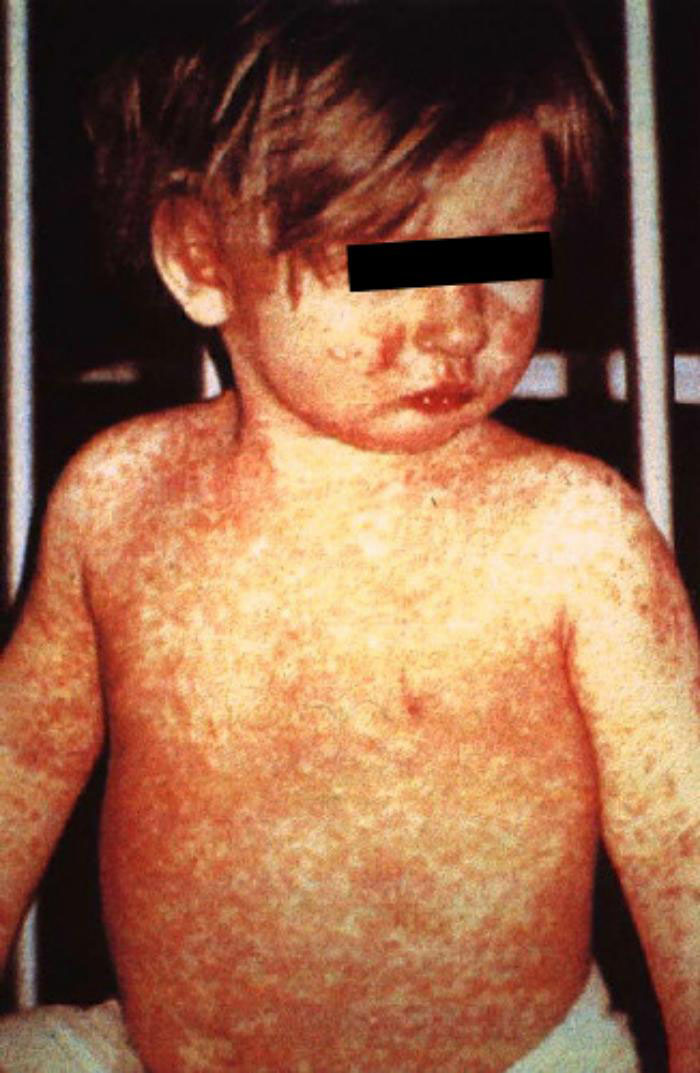
Measles
Medical Information
Measles is caused by a single-stranded, enveloped RNA virus, Measles morbillivirus. There is only one strain (i.e., serotype). The virus is classified as a member of the family Paramyxoviridae.
Humans are the only natural hosts of measles virus.1
Measles Infection
Measles is very contagious, and can spread through the air or through contact with infected respiratory secretions and saliva. Infected people can release the virus into the air when they breathe, cough, or sneeze. The measles virus can remain infectious on surfaces for several hours-typically up to about two hours. As infectious particles enter the air and settle on surfaces, anyone close to an infectious person and who is not immune can become infected.
The first sign of measles is usually a high fever, which begins about 10-12 days after exposure to the virus and lasts 4-7 days. A runny nose, cough, red and watery eyes, and white spots inside the cheeks can develop in the initial stage. After several days, a rash erupts, usually beginning on the face and upper neck. Over about three days, the rash spreads, eventually reaching the hands and feet. The rash lasts for 5-6 days. On average, the rash occurs 14 days after exposure to the virus (within a range of 7-21 days).
Infected people, including children and adults, can spread the measles virus for several days before they develop a rash. People are most infectious while they have symptoms such as fever and cough, and most people remain infectious for several days once the rash appears. However, some immunocompromised people (i.e., those with weakened immune systems) may be able to spread the virus until they fully recover. People who develop measles-like symptoms after vaccination are not typically able to spread measles to others.
Dangers to Workers Who Are Pregnant or May Become Pregnant
Measles can be especially hazardous for workers who are or may become pregnant because it may cause pregnant women to give birth prematurely. Babies born to infected mothers may have a low birth weight, which is sometimes associated with serious health problems for the infant.
Because of the risk of adverse health effects associated with measles infection during pregnancy, the Centers for Disease Control and Prevention (CDC) recommends that anyone without immunity get the measles, mumps, and rubella (MMR) vaccine at least one month before becoming pregnant. The MMR vaccine may cause complications if administered during pregnancy. Accordingly, pregnancy is included among conditions that preclude vaccination (i.e., contraindications). Healthcare providers are best equipped to provide individualized information to workers who are or may become pregnant and who have questions or concerns about measles vaccination and immunity.
Vaccines and Treatment
Most people born in the United States since the early 1970s have been vaccinated for measles, as CDC recommends children get two doses of MMR vaccine, with the first dose at 12–15 months of age and the second dose at 4–6 years of age. Adults who did not receive the vaccine as children can still be vaccinated.
According to CDC, the MMR vaccine is very safe and effective. Two doses of the MMR vaccine are about 97% effective at providing immunity to measles (i.e., immunogenicity); one dose is about 93% effective. Because measles is highly contagious, about 90% of unvaccinated people exposed to measles will get the disease.
Vaccine-related complications are typically infrequent and, when they do occur, mild (e.g., fever, rash). CDC has found no evidence that any vaccine causes autism or autism spectrum disorder (ASD).2 By definition of ASD as a developmental disability under the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders (DSM-5), adults, including those who receive the MMR or any other vaccine, do not develop autism later in life; cases of ASD diagnosed in adults have been present since childhood but not recognized until later in life.
The MMR vaccine is also effective at preventing measles when administered to a susceptible person within 72 hours following exposure. Because of the short period after exposure during which the vaccine is effective, healthcare providers may opt to give exposed individuals who may not be immune to the virus an additional dose of vaccine rather than waiting for laboratory testing to determine immunity. Unless otherwise contraindicated, extra doses of MMR are not harmful.
Immunoglobulin (IG) may prevent or lessen the severity of measles disease in susceptible people when given within six days following exposure and may be recommended for people who have contraindications for receiving the vaccine. (Note: healthcare providers should consult CDC recommendations for post-exposure prophylaxis, including guidelines for administering the MMR vaccine or IG, but not both.)
Testing for Measles
CDC recommends that healthcare professionals obtain a throat swab (specifically, from the nasopharynx) and blood specimen from all patients with clinical features compatible with measles (i.e., symptoms of the disease).
Healthcare professionals can contact their state and/or local health department to determine where to submit specimens and how to ship them. For information on sending specimens to the CDC from within the United States, please visit the CDC page on specimen collection, storage, and shipment.
1 U.S. Department of Health and Human Services (HHS), Centers for Disease Control and Prevention (CDC). Measles (Rubeola) – For Healthcare Professionals.
2 Hamborsky, J., Kroger, A., & Wolfe, C.S. (2015). Pinkbook: Epidemiology and Prevention of Vaccine-Preventable Diseases. Atlanta, GA: U.S. Department of Health and Human Services (HHS), Centers for Disease Control and Prevention (CDC).