Ergonomics Program Management Guidelines For Meatpacking Plants
U.S. Department of Labor
Robert B. Reich, Secretary
Occupational Safety and Health Administration
Joseph A. Dear, Assistant Secretary
OSHA 3123
1993 (Reprinted)
The information contained in this publication is not considered a substitute for any provisions of the Occupational Safety and Health Act of 1970 or for any standards issued by OSHA.
Material contained in this publication is in the public domain and may be reproduced, fully or partially, without the permission of the Federal Government. Source credit is requested but not required.
This information will be made available to sensory impaired individuals upon request. Voice phone: (202) 219-8615; Telecommunications Device for the Deaf (TDD) message referral phone: 1-800-326-2577
CONTENTS
INTRODUCTION
- MANAGEMENT COMMITMENT AND EMPLOYEE INVOLVEMENT
- Commitment by Top Management
- Written Program
- Employee Involvement
- Regular Program Review and Evaluation
- PROGRAM ELEMENTS
- Worksite Analysis
- Hazard Prevention and Control
- Engineering Controls
- Work Practice Controls
- Personal Protective Equipment
- Administrative Controls
- Medical -Management
- Training and Education
- General Training
- Job-Specific Training
- Training for Supervisors
- Training for Managers
- Training for Engineers and Maintenance Personnel
- DETAILED GUIDANCE AND EXAMPLES
- Recommended Worksite Analysis Program for Ergonomics
- Information Sources
- Screening Surveys
- Ergonomic Job Hazard Analyses
- Periodic Ergonomic Surveys
- Hazard Prevention and Control: Examples of Engineering Controls for the Meat Industry
- Work Station Design
- Design of -Work Methods
- Tool Design and Handles
- Medical Management Program for the Prevention and Treatment of Cumulative Trauma Disorders in meatpacking Establishments
- General
- Trained and Available Health Care Providers
- Periodic Workplace Walkthrough
- Symptoms Survey
- Compile a List of Light-Duty Jobs
- Health Surveillance
- Employee Training and Education
- Encourage Early Reporting of Symptoms
- Protocols for Health Care Providers
- Evaluation, Treatment, and Followup of CTDs
- Recordkeeping-OSHA Recordkeeping Forms
- Monitor Trends
- Recommended Worksite Analysis Program for Ergonomics
Exhibit 1- Symptoms Survey Checklist
Exhibit 2- Screening Tests
Exhibit 3- Upper Extremity Cumulative Trauma Disorders Algorithm
Selected Bibliography
Glossary
Questions and Answers
Other Sources of OSHA Assistance
States with Approved Plans
OSHA Consultation Project Directory
OSHA Area Offices
OSHA and BLS Regional Offices
Ergonomics Program Management Guidelines for Meatpacking Plants
Introduction
In recent years, there has been a significant increase in the reporting of cumulative trauma disorders (CTDs) and other work-related disorders due to ergonomic hazards. CTDs account for an increasingly large percentage of workers' compensation costs each year, and they represent nearly half of the occupational illnesses reported in the annual Bureau of Labor Statistics (BLS) survey. Much of the increase in CTDs is due to changes in process and technology that expose employees to increased repetitive motion and other ergonomic risk factors; some may be attributed to increased awareness-by industry, labor, and government-and reporting of these disorders.
Finding solutions to the problems posed by ergonomic hazards may well be the most significant workplace safety and health issue of the 1990s. The Occupational Safety and Health Administration (OSHA) is committed to a variety of efforts to address this issue.
The effective management of worker safety and health protection includes all work-related hazards, whether or not they are regulated by specific federal standards. The Occupational Safety and Health Act of 1970 (OSH Act) clearly states that the general duty of all employers is to provide their employees with a workplace free from recognized serious hazards. This includes the prevention and control of ergonomic hazards.
OSHA is therefore providing information and guidance on ergonomics program management to assist employers in meeting their responsibilities under the OSH Act. In January 1989, OSHA published voluntary, general Safety and Health Program Management Guidelines (Federal Register, Vol. 54, No. 16, January 26, 1989, pp. 3904-3916), which are recommended to all employers as a foundation for their safety and health programs and as a framework for their ergonomics programs. In addition, OSHA has developed the following ergonomics program management guidelines specifically for the meatpacking industry.
In this context, it is important to emphasize that this is not a new standard or regulation. We expect employers to implement effective ergonomics programs, adapted to their particular workplaces, containing the major elements described in the guidelines. OSHA's field inspection staff have been instructed that failure to implement the guidelines is not in itself a violation of the General Duty Clause of the OSH Act. The guidelines provide information on the steps employers should take (1) to determine if they have ergonomic-related problems in their workplaces, (2) to identify the nature and location of those problems, and (3) to implement measures to reduce or eliminate them.
Why meatpacking? Most importantly, CTDs are particularly prevalent in the meatpacking industry. Although ergonomic hazards are by no means confined to meatpacking, the incidence and severity of CTDs and other workplace injuries and illnesses in this industry demand that effective programs be implemented to protect workers from these hazards. These should be part of the employer's overall safety and health management program.
The publication and distribution of these guidelines is OSHA's first step in assisting the meatpacking industry in implementing a comprehensive safety and health program including ergonomics. OSHA's approach focuses on ergonomics, but also will cover the full range of safety and health hazards found in meatpacking. It will be a coordinated effort involving research, information, training, cooperative programs, and enforcement. The program will cover the "red meat" packing industry, Standard Industrial Classification (SIC) code 2011.
OSHA seeks the cooperation and commitment of you, the employer, in making this program an effective effort for occupational safety and health. It is essential that employers in SIC 2011 and related industries adopt an appropriately comprehensive program for addressing ergonomic hazards.
OSHA has developed its guidelines based on the best available scientific evidence, advice from the National Institute for Occupational Safety and Health (NIOSH), medical literature, and its experience in enforcement. They closely resemble the substance of settlement agreements with large meatpacking firms. These guidelines are intended to aid employers in implementing their programs. They are divided into three primary sections: (I) a discussion of the importance of management commitment and employee involvement, (II) recommended program elements, and (III) essential, detailed guidance and examples for the program elements. These elements are currently being implemented by leading employers voluntarily or by others, through settlement agreements with OSHA following enforcement actions. They are based on technical discussions and recommendations from NIGSH, representatives of the meat industry, employee representatives in the industry, and other*sources.
The four recommended program elements are (1) worksite analysis, (2) hazard prevention and control, (3) medical management and (4) training and education. While all of these elements should play a part in every employer's program, the one that should receive first attention is worksite analysis-finding out what actual or potential hazards now exist in your facility. This should be a careful, step-by-step look at your workplace to find out where hazards leading to CTDs exist. For smaller employers, OSHA does not believe a complicated effort should be necessary. Look at your injury/illness records, review any workers' compensation claims. look at the work as it is being done and ask questions of employees to see if there are ergonomic problems. Identify the jobs that appear to have the problems, and determine if those jobs involve ergonomic risk factors.
You should then take whatever measures are appropriate- including those set forth in the guidelines-to address the problems found, if any. If no problems exist, you should keep on with your current efforts to maintain a safe and healthful workplace.
In reading the guidelines, employers should be aware that the program elements are intended to be adapted, as appropriate, to the size and circumstances of the workplace. When OSHA visits a meatpacking plant, it does not expect a small facility to have the same type of hazard prevention program or medical management program as a large plant. The guidelines provide a general framework for action by employers and employees. Their flexibility allows for the incorporation of changes in technology and other advancements as they become available.
OSHA recognizes that small employers, in particular, may not have the need for as comprehensive a program as would result from implementation of every action and strategy described in these guidelines. There are numerous differences between large and small employers in the meatpacking industry-in types of operations, mechanization, and the degree of specialization in employee tasks. Accordingly, many small employers will not find the same extent of CTDs in their workplaces as their much larger counterparts.
Additionally, OSHA also realizes that many small employers may need assistance in implementing an appropriate ergonomics program. That is why we are emphasizing the availability of the free OSHA consultation service for smaller employers. The consultation service is independent of OSHA's enforcement activity and will be making special efforts to provide help in the meatpacking program. A directory of the consultation project offices in each State is included at the end of the guidelines. Also included is a section of Questions and Answers that are designed to respond to concerns employers may have.
The goal of any safety and health program is to prevent injuries and illnesses by removing their causes. For ergonomic hazards, this goal is achieved through taking steps to eliminate or materially reduce worker exposure to conditions that lead to cumulative trauma disorders and related injuries and illnesses.
The science of ergonomics seeks to adapt the job and workplace to the worker by designing tasks and tools that are within the worker's capabilities and limitations. Experience has shown that instituting programs in ergonomics has reduced cumulative trauma disorders and. often, improved productivity.
OSHA, therefore, looks to employers in the meatpacking industry to demonstrate that they are meeting their general duty under the OSH Act by evaluating the extent of the CTD's and ergonomic hazards in their workplaces, and by implementing appropriate, systematic programs to resolve them.
I. MANAGEMENT COMMITMENT AND EMPLOYEE INVOLVEMENT
Commitment and involvement are complementary and essential elements of a sound safety and health program. Commitment by management provides the organizational resources and motivating force necessary to deal effectively with ergonomic hazards.
Employee involvement and feedback through clearly established procedures are likewise essential, both to identify existing and potential hazards and to develop and implement an effective way to abate such hazards.
A. Commitment by Top Management
The implementation of an effective ergonomics program includes a commitment by the employer to provide the visible involvement of top management, so that all employees, from management to line workers, fully understand that management has a serious commitment to the program. An effective program should have a team approach, with top management as the team leader, and should include the following:
- Management's involvement demonstrated through personal concern for employee safety and health by the priority placed on eliminating the ergonomic hazards.
- A policy that places safety and health on the same level of importance as production. The responsible implementation of this policy requires management to integrate production processes and safety and health protection to assure that this protection is part of the daily production activity within each facility.
- Employer commitment to assign and communicate the responsibility for the various aspects of the ergonomics program so that all managers, supervisors, and employees involved know what is expected of them.
- Employer commitment to provide adequate authority and resources to all responsible parties, so that assigned responsibilities can be met.
- Employer commitment to ensure that each manager, supervisor, and employee responsible for the ergonomics program in the workplace is accountable for carrying out those responsibilities.
B. Written Program
Effective implementation requires a written program for job safety & health and ergonomics that is endorsed and advocated by the highest level of management and that outlines the employer's goals and plans. This written program should be suitable for the size and complexity of the workplace operations, and should permit these guidelines to be applied to the specific situation of each plant.
The written program should be communicated to all personnel, as it encompasses the total workplace, regardless of number of workers employed or the number of work shifts. It should establish clear goals, and objectives to meet those goals, that are communicated to and understood by all members of the organization.
The written program should include the earliest feasible implementation dates for completion of each program element.
C. Employee Involvement
An effective program includes a commitment by the employer to provide for and encourage employee involvement in the ergonomics program and in decisions that affect worker safety and health, including the following:
- An employee complaint or suggestion procedure that allows workers to bring their concerns to management and provide feedback without fear of reprisal.
- A procedure that encourages prompt and accurate reporting of signs and symptoms of CTDs by employees so that they can be evaluated and, if warranted, treated.
- Safety and health committees that receive information on ergonomic problem areas, analyze them, and make recommendations for corrective action.
- Ergonomic teams or monitors with the required skills to identify and analyze jobs for ergonomic stress and recommend solutions.
D. Regular Program Review and Evaluation
Procedures and mechanisms should be developed to evaluate the implementation of the ergonomic program and to monitor progress accomplished. Top management should review the program regularly -- semiannual reviews are recommended -- to evaluate success in meeting its goals and objectives. Evaluation techniques include methods such as the following:
- Analysis of trends in injury/illness rates.
- Employee surveys.
- Before and after surveys/evaluations of job/worksite changes
- Review of results of plant evaluations.
- Up-to-date records or logs of job improvements tried or implemented.
The results of management's review should be a written progress report and program update, which should be shared with all responsible parties and communicated to employees. New or revised goals arising from the review-identifying jobs, processes, and departments-should be shared with all workers. Any deficiencies should be identified and corrective action taken.
Managers, supervisors, and employees should review the program frequently to reevaluate goals and objectives and discuss changes. Regular-e.g., quarterly- meetings should be held on the progress of ergonomic issues. These should include managers, supervisors, and employees who review the goals and objectives identified and discuss changes in the program.
II. PROGRAM ELEMENTS
An effective occupational safety and health program to address ergonomic hazards in the meatpacking industry includes the following four major program elements: worksite analysis, hazard prevention and control, medical management, and training and education.
A. Worksite Analysis
Worksite analysis identifies existing hazards and conditions, operations that create hazards, and areas where hazards may develop. This also includes close scrutiny and tracking of injury and illness records to identify patterns of traumas or strains that may indicate the development of CTDs. (A recommended worksite analysis program for ergonomics is provided in Section III. A.)
The objectives of worksite analysis, then, are to recognize, identify, and correct ergonomic hazards.
- The first step in implementing the analysis program should be a review and analysis of injury and illness records to accomplish the following:
- Analyze safety, and insurance including the OSHA-200 log and information compiled through the medical management program, for evidence of cumulative trauma disorders. This process should involve health care providers to ensure confidentiality of patient records.
- Identify and analyze any apparent trends relating to particular departments, process units, job titles, operations, or work stations. (For a complete discussion, see Sections III. A. and C.)
- The worksite analysis should use a systematic method, such as the one provided in Section III. A., to identify those work positions needing a quantitative analysis of ergonomic hazards. This analysis should do the following:
- Use an ergonomic checklist that includes components such as posture, force, repetition, vibration, and various upper extremity factors. (See Section III. A.)
- Identify those work positions that put workers at risk of developing CTDs.
- Verify low risk factors for light duty or restricted activity work positions.
- Determine if risk factors for a work position have been reduced or eliminated to the extent feasible.
- Provide the results of such analyses to health care for use in assigning "light duty " jobs. (See Section 111. C. for discussion of these types of jobs.)
- Apply to all planned, new. and modified facilities, processes, materials, and equipment to ensure that workplace changes contribute to reducing or eliminating ergonomic hazards.
- The analysis of ergonomics hazards should be routinely performed and documented by a qualified person-ideally, an ergonomist; trained plant engineers, managers, health care providers, and affected employers should also contribute to the process.
- Periodic surveys of the worksite should be conducted-ar least annually, or whenever operations change- to identify new or previously unnoticed risk factors and deficiencies or failures in work practices or engineering controls, and to assess the effects of changes in the work processes.
Effective programs require a reliable system for employees to notify management about conditions that appear to be ergonomic hazards and to utilize their insight to determine appropriate work practice and engineering controls. This could be begun by a questionnaire on ergonomic problems and issues and maintained through an active safety and health committee or other forms of regular employee participation (e-g., a complaint log or suggestion book).
NOTE: After conducting a worksite analysis appropriate for the size and conditions of the workplace, the employer may find that there are no significant ergonomic hazards or resulting CTDs in the establishment. If there are no hazards, the employer need not implement the other program elements recommended by the guidelines. The employer should, however, continue current efforts to ensure workplace safety and health and should monitor changes in the workplace which might include ergonomic hazards.
B. Hazard Prevention and Control
Once ergonomic hazards are identified through :he systematic worksite analysis discussed above, the next step is to design measures to prevent or control these hazards. Thus, a system for hazard prevention and control is the second major program element for an effective ergonomics program.
Ergonomic hazards are prevented primarily by effective design of the workstation, tools, and job. To be effective, an employer's program should use appropriate engineering and work practice controls, personal protective equipment, and administrative controls to correct or control ergonomic hazards, including those identified in the following paragraphs:
- Engineering Controls
Engineering techniques, where feasible, are the preferred method of control. The focus of an ergonomics program is to make the job fit the person, not to force the person to fit the job. This can be accomplished by designing or modifying the work station, work methods, and tools to eliminate excessive exertion and awkward postures and to reduce repetitive motion.- Work Station Design. Work stations should be designed to accommodate the persons who actually work on a given job; it is not adequate to design for the "average" or typical worker.
Work stations should be easily adjustable and either designed or selected to fit a specific task, so they are comfortable for the workers using them.
The work space should be large enough to allow for the full range of required movements, especially where knives, saws, hooks, and similar tools are used. - Design of Work Methods. Work methods should be designed to reduce static, extreme, and awkward postures: repetitive motion; and excessive force. Work method design addresses the content of tasks performed by the workers. It requires analysis of the production system to design or modify tasks to eliminate stressors.
- Tool and Handle Design. Tools and handles, if well-designed, reduce the risk of CTDs.
- Work Station Design. Work stations should be designed to accommodate the persons who actually work on a given job; it is not adequate to design for the "average" or typical worker.
For any tool, a variety of sizes should be available to achieve a proper fit and reduce ergonomic risk. The appropriate tool should be used to do a specific job. Tools and handles should be selected to eliminate or minimize the following stressors:
- Chronic muscle contraction or steady force.
- Extreme or awkward finger/hand/arm positions.
- Repetitive forceful motions.
- Tool vibration.
- Excessive gripping. pinching, pressing with the hand and fingers.
For examples of engineering controls achievable in the meat industry to eliminate extreme and awkward postures and excessive force and to reduce repetitive motion in the meat industry, see Section III. B.
- Work Practice Controls
An effective program for hazard prevention and control also includes procedures for safe and proper work that are understood and followed by managers, supervisors, and workers. Key elements of a good work practice program for ergonomics include proper work techniques, employee conditioning, regular monitoring, feedback, maintenance, adjustments and modifications and enforcement.- Proper Work Techniques. A program for proper work techniques, such as the following, includes appropriate training and practice time for employees:
- Proper cutting techniques, including work methods that improve posture arid reduce stress and strain on extremities.
- Good knife care, including steeling and the regular sharpening or steeling of knives.
- Correct lifting techniques (proper body mechanics).
- Proper use and maintenance of pneumatic and power tools.
- Correct use of ergonomically designed work stations and fixtures.
- New Employee Conditioning Period. Jobs in the meat industry will usually require conditioning, or break-in, periods, which may last several weeks. New and returning employees should be gradually integrated into a full workload as appropriate for specific jobs and individuals. Employees should be assigned to an experienced trainer for job training and evaluation during the break-in period. Employees reassigned to new jobs should also have a break-in period.
- Monitoring. Regular monitoring at all levels of operation helps to ensure that employees continue to use proper work practices. This monitoring should include a periodic review of the techniques in use and their effectiveness, including a determination of whether the procedures in use are those specified; if not, then it should be determined why changes have occurred and whether corrective action is necessary.
- Adjustments and Modifications. Modify work change. Such adjustments include changes in the following:
- Line speeds.
- Staffing at position
- Type, size, weight, or temperature of the product handled.
- Proper Work Techniques. A program for proper work techniques, such as the following, includes appropriate training and practice time for employees:
PPE should be selected with ergonomic stressors in mind. Appropriate PPE should be provided in a variety of sizes, should accommodate the physical requirements of workers and the job, and should not contribute to extreme postures and excessive forces. The following factors need to be considered when selecting PPE in the meat industry:
- Proper fit is essential. For example, gloves that are too thick or that fit improperly can reduce blood circulation and sensory feedback, contribute to slippage, and require excessive grip strength. The same is true when excessive layers of gloves are used (e.g., rubber over fabric, over metal mesh, over cotton). The gloves in use should facilitate the grasping of the tools and knives needed for a particular job while protecting the worker from injury.
- Protection against extreme cold (less than 40 degrees Fahrenheit in most meat operations) is necessary to minimize stress on joints.
- Braces, splints, back belts, and other similar devices are not PPE. See Section III. C., "Medical Management Program ."
- Other types of PPE that maybe selected for use(e.g., arm guards) should not increase ergonomic stressors.
- Administrative Controls
A sound overall ergonomics program includes administrative controls that reduce the duration, frequency, and severity of exposures to ergonomic stressors.- Examples of administrative methods include the following:
- Reducing the total number of repetitions per employee by such means as decreasing production rates and limiting overtime work.
- Providing rest pauses to relieve fatigued muscle-tendon groups. The length of time needed depends on the task's overall effort and total cycle time.
- Increasing the number of employees assigned to a task to alleviate severe conditions, especially in lifting heavy objects.
- Using job rotation, used with caution and as a preventive measure, not as a response to symptoms. The principle of job rotation is to alleviate physical fatigue and stress of a particular set of muscles and tendons by rotating employees among use different muscle-tendon groups. If rotation is utilized, the job analyses must be reviewed by a qualified person to ensure that the same muscle-tendon groups are not used.
- Providing sufficient numbers of standby/relief personnel to compensate for foreseeable upset conditions on the line (e.g., loss of workers).
- Job enlargement-see the guidance on "Design of Conservative treatment. Work Methods" given in Sections 11. B. 1. and 111. B.
- Effective programs for facility, equipment, and tool maintenance to minimize ergonomic stress include the following measures:
- A preventive maintenance program for mechanical and power tools and equipment, such as powered knives and saws. to verify that they are in proper working order and within original manufacturer's specifications. This may include vibration monitoring.
- Perform maintenance regularly and whenever workers report suspected problems. Sufficient numbers of spare tools should be available to facilitate regular maintenance.
- A specific knife sharpening program. Sharp knives should be readily available.
- Effective housekeeping programs to minimize slippery work surfaces and related hazards such as slips and falls.
- Examples of administrative methods include the following:
C. Medical Management
Implementation of a medical management system is the third major element in the employer's ergonomics program. Proper medical management is necessary both to eliminate or materially reduce the risk of development of CTD signs and symptoms through early identification and treatment and to prevent future problems through development of information sources.
Thus, an effective medical management program for CTDs is essential: to the success of any employer's ergonomics program. In an effective program, health care providers will be part of the ergonomic team, interacting and exchanging information routinely in order to prevent and properly treat CTDs.
The guidelines describe the elements of a medical management program for CTDs and related ergonomic issues to ensure early identification, evaluation, and treatment of signs and symptoms; and to aid in their prevention. Each plant should establish standard procedures for the medical management of work-related illnesses or injuries.
A physician or occupational health nurse (OHN) with training in the prevention and treatment of CTDs should supervise the program. Each work shift should have access to health care providers in order to facilitate treatment, surveillance activities, and recording of information. Where such personnel are not employed full-time, the part-time employment of appropriately trained health care providers is recommended.
The medical management program should address the following issues:
- Injury and illness recordkeeping.
- Early recognition and reporting.
- Systematic evaluation and referral.
- Conservative treatment.
- Conservative return to work.
- Systematic monitoring
- Adequate staffing and facilities.
Recommendations for medical management of CTDs are evolving rapidly, and health care providers should monitor developments on the subject.
(See Section 111. C. for a full description of a recommended program for the medical management of CTDs in meatpacking establishments.)
D. Training and Education
The fourth major program element for an effective ergonomics program is training and education. The purpose of training and education is to ensure that employees are sufficiently informed about the ergonomic hazards to which they may be exposed and thus are able to participate actively in their own protection. Employees should be adequately trained about the employer's ergonomics program.
Training and education are critical components of an ergonomics program for employees potentially exposed to ergonomic hazards. Training allows managers, supervisors, and employees to understand ergonomic and other hazards associated with a job or production process, their prevention and control, and their medical consequences.
A training program should include the following individuals:
- All affected employees.
- Engineers and maintenance personnel.
- Managers.
- Health care providers.
The program should be designed and implemented by qualified persons. Appropriate special training should be provided for personnel responsible for administering the program.
The program should be presented in language and at a level of understanding appropriate for the individuals being trained. It should provide an overview of the potential risk of illnesses and injuries, their causes and early symptoms, the means of prevention, and treatment.
The program should also include a means for adequately evaluating its effectiveness. This might be achieved by using employee interviews, testing, and observing work practices, to determine of those who received the training understand the material and the work practices to be followed.
Training for affected employees should consist of both general and specific job training:
- General Training
Employees who are potentially exposed to ergonomic hazards should be given formal instruction on the hazards associated with their jobs and with their equipment. This includes information on the varieties of CTDs, what risk factors cause or contribute to them, how to recognize and report symptoms, and how to prevent these disorders. This instruction should be repeated for each employee as necessary. OSHA's experience indicates that, at minimum, annual retraining is advisable.
- Job-Specific Training
New employees and reassigned workers should receive an initial orientation and hands-on training prior to being placed in a full-production job. Training lines may be used for this purpose. Each new hire should receive a demonstration of the proper use of and procedures for all tools and equipment. The initial training program should include the following:
- Care, use, and handling techniques for knives.
- Use of special tools and devices associated with individual work stations.
- Use of appropriate guards and safety equipment, including personal protective equipment.
- Use of proper lifting techniques and devices.
On-the-job training should emphasize employee development and use of safe and efficient techniques. (See also the section on "New Employee Conditioning Period" under Work Practice Controls, 11. B. 1. b.)
- Training for Supervisors
Supervisors are responsible for ensuring that employees follow safe work practices and receive appropriate training to enable them to do this. Supervisors therefore should undergo training comparable to that of the employees, and such additional training as will enable them to recognize early signs and symptoms of CTDs to recognize hazardous work practices to correct such practices, and to reinforce the employer's ergonomic program, especially through the ergonomic training of employees as may be needed.
- Training for Managers
Managers should be aware of their safety and health responsibilities and should receive sufficient training pertaining to ergonomic issues at each work station and in the production process as a whole so that they can effectively carry out their responsibilities.
- Training for Engineers and Maintenance Personnel
Plant engineers and maintenance personnel should be trained in the prevention and correction of ergonomic hazards through job and work station design and proper maintenance, both in general and as applied to the specific conditions of the facility.
III. DETAILED GUIDANCE AND EXAMPLES
- Recommended Worksite Analysis Program for Ergonomics
General. While complex analyses are best performed by a professional ergonomist, the "ergonomic team" or any qualified person-can use this program to identify stressors in the workplace. The purpose of the outline that follows is to give a starting point for finding and eliminating those tools, techniques, and conditions which may be the source of ergonomic problems. In addition to analyzing current workplace conditions, planned changes to existing and new facilities, processes, materials, and equipment should be analyzed to ensure that changes made to enhance production will also reduce or eliminate the risk factors.
As has been emphasized elsewhere, this program should be adapted to each workplace. It is based on the sources listed in the Selected Bibliography.
Outline. The discussion of the recommended program for worksite analysis is divided into for main categories:- Gathering information from available sources;
- Conducting baseline screening surveys to determine which jobs need a closer analysis;
- Performing ergonomic job hazard analyses of those work stations with identified risk factors; and -- after implementing control measures --
- Conducting periodic surveys and followup to evaluate changes.
- Information Sources
- Records Analysis and Tracking. The essential first step in worksite analysis is to develop the information necessary to identify ergonomic hazards in the workplace. (See Section 11. A.) Existing medical, safety, and insurance records, including OSHA-200 logs, should be analyzed for evidence of injuries or disorders associated with CTDs. Health care providers should participate in this process to ensure confidentiality of patient records.
(NOTE: See also Section III. C., Medical Management Program.) - Incidence Rates. Incidence rates for upper extremity disorders and/or back injuries should be calculated by counting the incidences of CTDs and reporting the incidences per 100 full time workers per year per facility.
- Records Analysis and Tracking. The essential first step in worksite analysis is to develop the information necessary to identify ergonomic hazards in the workplace. (See Section 11. A.) Existing medical, safety, and insurance records, including OSHA-200 logs, should be analyzed for evidence of injuries or disorders associated with CTDs. Health care providers should participate in this process to ensure confidentiality of patient records.
Incidence = (number of new cases/yr) x (200,000 work hrs) per facility* Rate number of hours worked/facility/yr
*The same method should be applied to departments, production lines, or job types within the facility.
- Screening Surveys
The second step in worksite analysis under an effective ergonomics program is to conduct baseline screening surveys. Detailed baseline screening surveys identify jobs that put employees at risk of developing CTDs. If the job places employees at risk of developing CTDs, an effective program will then require the ergonomic job hazard analysis described at Section 111. A. 3. below.- Checklist. The survey is performed with an ergonomic checklist. This checklist should include components such as posture, materials handling, and upper extremity factors. (The checklist should be tailored to the specific needs and conditions of the workplace. One example of an ergonomics checklist is provided by Putz-Anderson in Cumulative Trauma Disorders, p. 52; see Selected Bibliography. Other examples of checklists will be given in OSHA's forthcoming Ergonomics Program Management Guidelines for General Industry.)
- Ergonomic Risk Factors. Identification of ergonomic hazards is based on ergonomic risk factors: conditions of a job process, work station, or work method that contribute to the risk of developing CTDs. Not all of these risk factors will be present in every CTD-producing job, nor is the existence of one of these factors necessarily sufficient to cause a CTD.
- CTD Risk Factors. Some of the risk factors for CTDs of the upper extremities include the following:
- Repetitive and/or prolonged activities.
- Forceful exertions, usually with the hands (including pinch grips).
- Prolonged static postures.
- Awkward postures of the upper body, including reaching above the shoulders or behind the back, and twisting the wrists and other joints to perform tasks.
- Continued physical contact with work surfaces; e.g., contact with edges.
- Excessive vibration from power tools.
- Cold temperatures.
- Inappropriate or inadequate hand tools.
- Back Disorder Risk Factors. Risk factors for back disorders include items such as the following:
- Bad body mechanics such as (1) continued bending over at the waist; (2) continued lifting from below the knuckles or above the shoulders; and (3) twisting at the waist, especially while lifting.
- Lifting or moving objects of excessive weight or asymmetric size.
- Prolonged sitting, especially with poor posture.
- Lack of adjustable chairs, footrests, body supports, and work surfaces at work stations.
- Poor grips on handles.
- Slippery footing.
- Multiple Risk Factors. Jobs, operations, or work stations that have multiple risk factors have a higher probability of causing CTDs. The combined effect of several risk factors in the development of CTDs is sometimes referred to as "multiple causation."
- Ergonomic Job Hazard Analyses
At this point, the employer has identified-through the information sources and screening surveys discussed above-jobs that place employees at risk of developing CTDs. As an essential third step in the worksite analysis, an effective ergonomics program requires a job hazard analysis for each job so identified.
Job hazard analyses should be routinely performed by a qualified person for jobs that put workers at risk of developing CTDs. This type of analysis helps to verify lower risk factors at light duty or restricted activity work positions and to determine if risk factors for a work position have been reduced or eliminated to the extent feasible.- Work Station Analysis. An adequate analysis would be expected to identify all risk factors present in each studied job or workstation.
For upper extremities, three measurements of repetitiveness are the total hand manipulations per cycle, the cycle time, and the total manipulations or cycles per work shift.
Force measurements may be noted as an estimated average effort, and a peak force. They may be recorded as "light ," "moderate ," and "heavy." (See also Putz-Anderson, Selected Bibliography, pp. 57-59, for additional guidance on force measurements.)
Tools should be checked for excessive vibration. (See also NIOSH criteria document on hand/arm vibration, Selected Bibliography.)
The tools, personal protective equipment, and dimensions and adjustability of the work station should be noted for each job hazard analysis.
Finally, hand, arm, and shoulder postures and movements should be assessed for levels of risk. - Lifting Hazards. For manual materials handling, the maximum weight-lifting values should be calculated. (See the NIOSH Work Practices Guide for Manual Lifting, 1981, in the Selected Bibliography. for basic calculations. Note that this guide does not address lifting that involves twisting or turning motions.)
- Videotape Method. The use of videotape, where feasible, is suggested as a method for analysis of the work process. Slow-motion videotape or equivalent visual records of workers performing their routine job tasks should be analyzed to determine the demands of the task on the worker and how each worker actually performs each task.
NOTE: Ergonomic analysis is not complete without implementation of controls. Section III. B., which follows, offers examples of engineering controls and other methods that will be useful in reducing ergonomic hazards.
- Work Station Analysis. An adequate analysis would be expected to identify all risk factors present in each studied job or workstation.
- Periodic Ergonomic Surveys
The fourth step in worksite analysis is to conduct periodic review. Periodic surveys should be conducted, to identify previously unnoticed risk factors or failures or deficiencies in work practice or engineering controls. The "symptoms survey" described in Section III. C. is an effective tool in identifying jobs that require ergonomic job hazard analysis.
The periodic review process should also include the following:- Feedback and Followup. A reliable system should be provided so that employees can notify management about conditions which appear to be ergonomic hazards and to utilize their insight and experience to determine work practice and engineering controls. This might be initiated by an ergonomic questionnaire and be maintained through an active safety and health committee, or by employee participation with the "ergonomic team."
Reports of ergonomic hazards or signs and symptoms of potential CTDs should be investigated by ergonomic screening surveys and appropriate ergonomic hazard analyses in order to identify risk factors and controls. - Trend Analysis. Trends of injuries and illnesses related to actual or potential CTDs should be calculated, using several years of data where possible.
Trends should be calculated for several departments, process units, job titles, or work stations. These trends may also be used to determine which work positions are most hazardous and need to be analyzed by the qualified person.
Using standardized job descriptions, incidence rates may be calculated for work positions in successive years to identify trends. Using trend information can help to determine the priority of screening surveys and/or ergonomic hazard analyses.
- Feedback and Followup. A reliable system should be provided so that employees can notify management about conditions which appear to be ergonomic hazards and to utilize their insight and experience to determine work practice and engineering controls. This might be initiated by an ergonomic questionnaire and be maintained through an active safety and health committee, or by employee participation with the "ergonomic team."
B. Hazard Prevention and Control: Examples of Engineering Controls for the Meat Industry
Engineering solutions, where feasible, are the preferred method of control for ergonomic hazards. The focus of an ergonomics program is to make the job fit the person, not to make the person fit the job. This is accomplished by redesigning the work station, work methods, or tool to reduce the demands of the job, including high force, repetitive motion, and awkward postures. A program toward this end entails research into currently available controls and technology. It also includes provisions for utilizing new technologies as they become available and for in-house research and testing.
The following are examples of engineering controls that have been found to be effective and achievable in the industry.

- Work Station Design
Work stations should be designed to accommodate the persons who actually work on a given job; it is not adequate to design for the "average" or typical worker. Work stations should be easily adjustable and either designed or selected to fit a specific task: so that they are comfortable for the workers using them. The work space should be large enough to allow for the full range of required movements, especially where knives, saws, hooks, and similar tools are used.- EXAMPLES of methods for the reduction of extreme and awkward postures include the following:
- Adjustable fixtures and rotating cutting tables so that the position of the meat can be easily manipulated.
- Work stations and delivery bins that can accommodate the heights and reach limitations of various-sized workers.
- Work platforms that move up and down for operations such as splitters.
- EXAMPLES of methods for the reduction of excessive force in the meat industry include the following:
- Adjustable fixtures to allow cuts and movements to be made easily.
- Bins properly located so that workers do not have to toss products and by-products.
- Mechanical or powered assists to eliminate the use of extreme force.
- Suspension of heavy tools.
- An EXAMPLE of a means by which highly repetitive movements can be reduced is as follows:
- The use of diverging conveyors off the main line so that certain activities can be performed at slower rates.
- EXAMPLES of methods for the reduction of extreme and awkward postures include the following:
- Design of Work Methods
Traditional work method analysis considers static postures and repetition rates. This should be supplemented by addressing the force levels and the hand and arm postures involved. The tasks should be altered to reduce these and the other stresses identified with CTDs. The results of such analyses should be shared with the health care providers; e.g., to assist in compiling lists of "light-duty" and "high-risk" jobs.- EXAMPLES of methods for the reduction extreme and awkward postures include the following:
- Enabling the worker to perform the task with two hands instead of one.
- Conforming with the NIOSH Work Practices Guide for Manual Lifting
- EXAMPLES of methods to reduce excessive force include the following:
- The use of automation, such as automated deboners.
- The use of mechanical devices to aid in removing bones and in separating meat from bones, and for heavy lifting.
- Substitution of power tools where manual tools are now in use.
- The use of articulated arms and counter balances suspended by overhead racks to reduce the force needed to operate and control power tools.
- Ensuring that the meat to be processed is kept from freezing and is completely thawed.
- EXAMPLES of methods to reduce highly repetitive movements include the following:
- Increasing the number of workers performing a task. Lessening repetition by combining jobs with very short cycle times, thereby increasing cycle time. (Sometimes referred to as "job enlargement.")
- Using automation.
- Designing jobs to allow self-pacing, when feasible.
- Designing jobs to allow sufficient rest pauses.
- EXAMPLES of methods for the reduction extreme and awkward postures include the following:
- Tool Design and Handles
Attention should be paid to the selection and design of tools to minimize the risks of upper extremity CTDS and back injuries.
In any tool design, a variety of sizes should be available. EXAMPLES of criteria for selecting tools include the following:- Matching the type of tool or knife to the task.
- Designing or selecting the tool handle or knife so that extreme and awkward postures are minimized.
- Using knife or tool handles with textured grips in preference to those with ridges and grooves.
- Designing tools to be used by either hand or providing tools for both left- and right-handed workers.
- Using tools with triggers that depress easily and are activated by two or more fingers.
- Using handles and grips that distribute the pressure over the fleshy part of the palm, so that the tool does not dig into the palm.
- Designing tools for minimum weight; counter-balancing tools heavier than one or two pounds.
- Selecting pneumatic and power tools that exhibit minimal vibration and maintaining them in accordance with manufacturer's specifications, or with an adequate vibration monitoring program. Wrapping handles and grips with insulation material (other than wraps provided by the manufacturer for this purpose) is normally not recommended, as it may interfere with a proper grip and increase stress.
C. Medical Management Program for the Prevention and Treatment of Cumulative Trauma Disorders in Meatpacking Establishments
- General
As noted in several sections of these guidelines, an effective medical management program for cumulative trauma disorders (CTDs is essential to the success of an employer's ergonomic program in the meatpacking industry.
It is not the purpose of these guidelines to dictate medical practice for an employer's health care providers. Rather, they describe the elements of a medical management program for CTDs to ensure early identification, evaluation, and treatment of signs and symptoms; to prevent their recurrence; and to aid in their prevention. Medical management of CTDs is a developing field, and health care providers should monitor developments on the subject. These guidelines represent the best information currently available.
A physician or occupational health nurse (OHN) with training in the prevention and treatment of CTDs should supervise the program. Each work shift should have access to health care providers in order to facilitate treatment, surveillance activities, and recording of information. Where such personnel are not employed full-time, the part-time employment of appropriately trained health care providers is recommended.
In an effective ergonomics program, health care providers should be part of the ergonomics team, interacting and exchanging information routinely to prevent and properly treat CTDs. The major components of a medical management program for the prevention and treatment of CTDs are trained first-level health care providers, health surveillance, employee training and education, early reporting of symptoms, appropriate medical care, accurate recordkeeping, and quantitative evaluation of CTD trends throughout the plant.
For a definition of disorders associated with repeated trauma; also known as cumulative trauma disorders, see the Glossary. - Trained and Available Health Care Providers
Appropriately trained health care providers should be available at all times, and on an ongoing basis as part of the ergonomic program.
In an effective medical management program, first-level health care providers should be knowledgeable in the prevention, early recognition, evaluation, treatment and rehabilitation of CTDs, and in the principles of ergonomics, physical assessment of employees, and OSHA recordkeeping requirements. - Periodic Workplace Walkthrough
In an effective program, health care providers should conduct periodic, systematic workplace walkthrough's to remain knowledgeable about operations and work practices, to identify potential light duty jobs, and to maintain close contact with employees. Health care providers also should be involved in identifying risk factors for CTDs in the workplace as part of the ergonomic team.
These walkthrough surveys should be conducted every month or whenever a particular job task changes. A record should be kept documenting the date of the walkthrough, area(s) visited, risk factors recognized, and action initiated to correct identified problems. Followup should be initiated and documented to ensure corrective action is taken when indicated. - Symptoms Survey
Those responsible for the medical management program should develop a standardized measure of the extent of symptoms of work-related disorders for each area of the plant, to determine which jobs are exhibiting problems and to measure progress of the ergonomic program. (See Putz-Anderson, pp. 42-44, Selected Bibliography.)- Institute a Survey. A survey of employees should be conducted to measure employee awareness of work-related disorders and to report the location, frequency, and duration of discomfort. Body diagrams should be used to facilitate the gathering of this information.
Surveys normally will not include employees' personal identifiers; this is to encourage employee participation in the survey. Survey information should include information such as that discussed in Exhibit 1 (Symptoms Survey Checklist).
The survey is one method for identifying areas or jobs where potential CTD problems exist. The major strength of the survey approach is in collecting data on the number of workers that may be experiencing some form of CTD. Reported pain symptoms by several workers on a specific job would indicate the need for further investigation of that job. - Conduct the Survey Annually. Conducting the survey annually should help detect any major change in the prevalence, incidence, and/or location of reported symptoms.
- Institute a Survey. A survey of employees should be conducted to measure employee awareness of work-related disorders and to report the location, frequency, and duration of discomfort. Body diagrams should be used to facilitate the gathering of this information.
- Compile a List of Light-Duty Jobs
The ergonomist or other qualified person should analyze the physical procedures used in the performance of each job, including lifting requirements, postures, hand grips, and frequency of repetitive motion. (See Section 111. A. and Putz-Anderson, pp. 47073, Selected Bibliography.) Positions with ergonomic stress should be so labeled.
The ergonomist and health care providers should develop a list of jobs with the lowest ergonomic risk. For such jobs, the ergonomic risk should be described. This information will assist health care providers in recommending assignments to light or restricted duty jobs. The light duty job should therefore not increase ergonomic stress on the same muscle-tendon groups.
Health care providers should likewise develop a list of known high-risk jobs.
Supervisors should periodically review and update the lists. - Health Surveillance
- Baseline. The purpose of baseline health surveillance is to establish a base against which changes in health status can be evaluated, not to preclude people from performing work. Prior to assignment, all new and transferred workers who are to be assigned to positions involving exposure of a particular body part to ergonomic stress should receive baseline health surveillance.
[NOTE: The use of medical screening tests or examinations have not been validated as predictive procedures for determining the risk of a worker developing a CTD.]
These positions should be identified through the worksite analysis program discussed in Sections 11. A. and III. A. and from the list of known high-risk jobs compiled by the health care provider. The majority of employees in the meatpacking industry can be expected to be in high-risk jobs.
The baseline health surveillance should include a medical and occupational history, and physical examination of the musculoskeletal and nervous systems as they relate to CTDs. The examination should include inspection, palpation, range of motion (active, passive and resisted), and other pertinent maneuvers of the upper extremities and back. Examples of the pertinent maneuvers for the hands and wrists include Tinel's test, Phalen's test, and Finkelstein's test. (See Exhibit 2 of this Section.) Laboratory tests, X-rays, and other diagnostic procedures are not a routine part of the baseline assessment. - Conditioning Period Followup. New and transferred employees should be given the opportunity during a 4-to-6-week break-in period to condition their muscle-tendon groups prior to working at full capacity. (See Section 11. B. 2. of the guidelines on "Work Practice Controls.") Health care providers should perform a followup assessment of these workers after the break-in period (or after one month, if the break-in period is longer than a month) to determine if conditioning of the muscle-tendon groups has been successful; whether any reported soreness or stiffness is transient and consistent with normal adaptation to the job or whether it indicates the onset of CTD; and if problems are identified, what appropriate action and further followup are required.
- Periodic Health Surveillance. Periodic health surveillance - every 2 to 3 years - should be conducted on all workers who are assigned to positions involving exposure of a particular body part to ergonomic stress. The content of this assessment should be similar to that outlined for the baseline. The worker's medical and occupational history should be updated.
- Documentation. gathered on workers as a result of health surveillance should be documented and filed in individual employee medical records.
- Baseline. The purpose of baseline health surveillance is to establish a base against which changes in health status can be evaluated, not to preclude people from performing work. Prior to assignment, all new and transferred workers who are to be assigned to positions involving exposure of a particular body part to ergonomic stress should receive baseline health surveillance.
- Employee Training and Education
Health care providers should participate in the training and education of all employees, including supervisors and other plant management personnel, on the different types of CTDs and means of prevention, causes, early symptoms and treatment of CTDs. This information should be reinforced during workplace walkthroughs and the individual health surveillance appointments. All new employees should be given such education during orientation. This demonstration of concern and the distribution of information should facilitate the early recognition of CTDs prior to the development of more severe and disabling conditions and increase the likelihood of compliance with prevention and treatment. - Encourage Early Report of Symptoms
Employees should be encouraged by health care providers and supervisors to report early signs and symptoms of CTDs to the in-plant health facility. This allows for timely and appropriate evaluation and treatment without fear of discrimination or reprisal by employers. It is important to avoid any potential disincentives for employee reporting, such as limits on the number of times an employee may visit the health unit. - Protocols for Health Care Providers
Health care providers should use written protocols for health surveillance and the evaluation, treatment, and followup of workers with signs or symptoms of CTDs. The protocols be prepared by a qualified health care provider. These protocols should be available in the plant health facility. Additionally, the protocols should be reviewed and updated annually and/or as state-of-the-art evaluation and treatment of these conditions changes. An example algorithm for the evaluation and treatment of upper extremity CTDs is included as Exhibit 3 of this Section. The date of review and signature of the reviewer should appear on each protocol. - Evaluation, Treatment, and Followup of CTD
If CTDs are recognized and treated appropriately early in their development, a more serious condition likely can be prevented; therefore, a good medical management program that seeks to identify and treat these disorders early is important. The following systematic approach, in general outline, is recommended in evaluating and following workers who report to the health unit.- Screening Assessment. Upon the employee's presentation of symptoms, the health care provider's screening assessment should include obtaining a history from the worker to identify the location, duration and onset of pain, discomfort, swelling, tingling and/or numbness, and associated aggravating factors. A brief, non-invasive screening examination for the evaluation of CTDs consists of inspection, palpation, range of motion testing, and various applicable maneuvers. (See Barbara Silverstein, Evaluation of Upper Extremity and Low Back, Selected Bibliography.)
(1)Based on the severity of symptoms and physical signs, the OHN or other health care provider should decide whether to initiate conservative treatment and/or to refer promptly to a physician for further evaluation. For example, an employee experiencing pain with a positive physical sign, such as positive Tinel's, Phalen's, or Finkelstein's tests, should be referred for physician evaluation. (See Exhibits 2 and 3 of this Section.)
(2) If mild symptoms and no physical signs are present, conservative treatment is recommended. Examples include the following:- Applying heat or cold. Ice is used to treat overuse strains and muscle/tendon disorders for relief of pain and swelling, thus allowing more mobility. Ice decreases the inflammation associated with CTDs even if no overt signs of inflammation (redness, warmth, or swelling) are present. The use of ice may be inappropriate for Raynaud's disease (vibration syndrome), rheumatoid arthritis, and diabetic conditions. Heat treatments should be used only for muscle strains where no physical signs of inflammation are present. (See Putz-Anderson, p. 125, Selected Bibliography.)
- Nonsteroidal anti-inflammatory agents. These agents may be helpful in reducing inflammation and pain. Examples of these types of agents include aspirin and ibuprofen.
- Special exercise. If active exercises are utilized for employees with CTDs, they should be administered under the supervision of the OHN or physical therapist. If these active exercises are performed improperly, they may aggravate the existing condition. (See Putz-Anderson, p. 126, Selected Bibliography.)
- Splints. A splint may be used to immobilize movement of the muscles, tendons, and nerves. Splints should not be used during working activities unless it has been determined by the OHN and ergonomist that no wrist deviation or bending is performed on the job. Splinting can result in a weakening of the muscle, loss of normal range of motion due to inactivity, or even greater stress on the area if activities are carried out while wearing the splint.
- Followup Assessment After Two Days. (1) If the condition has resolved, reinforce good work practices and encourage the employee to return to the health facility if there are problems.
(2) If the condition has improved but is not resolved, continue the above treatment for approximately 2 days and reevaluate.
(3) If the condition is unchanged or worse, check compliance with the prescribed treatment and perform a screening examination. (See also section above, "Screening Assessment," for screening examination.)
If the screening examination is positive, or if the condition is worse, refer the worker to the company physician, and seek reassignment of the employee to a light or restricted duty position.
If the screening examination is negative for physical signs, but the condition is unchanged, continue conservative treatment.
(4) A job reassignment must be chosen with knowledge of whether the new task will require the use of the injured tendons, or place pressure on the injured nerves. Inappropriate job reassignment can continue to injure the inflamed tendon or nerve, which can result in permanent symptoms or disability. The appropriate light duty job can be selected from the list maintained by the health care provider.
Restricted or light duty jobs are one of the most helpful treatments for CTDs. These jobs, if properly selected, allow the worker to perform while continuing to ensure recovery. Some CTDs require weeks (or months, in rare cases) of reduced activity to allow for complete recovery. - Followup Assessment After Six Days. ( 1 ) After about 6 days, if the condition has now resolved, reinforce good work practices and encourage the employee to return to the health facility with problems.
(2) If the condition has improved but is not resolved, continue the above treatment for approximately 2 more days and reevaluate.
(3) If the condition is unchanged or worse, check compliance with prescribed treatment and perform a screening examination. If the screening examination is positive. refer the worker to the company physician. - Followup After Eight Days. (1) If, after about 8 days, the condition has now resolved, reinforce good work practices and encourage the employee to return to the health facility with problems.
(2) If the condition has not resolved within approximately 8 days, refer to the company physician automatically. - Other Considerations. (1) If an employee misses a scheduled reevaluation, the health care provider should contact the employee to assess the condition within approximately 5 days of the last presentation.
(2) The referring physicians or health care providers should be furnished with a written description of the ergonomic characteristics of the job of the worker who is being referred.
(3) Surgery. Recommendations for surgery should be referred for a second opinion.
If surgery is performed, an appropriate amount of time off work is essential to allow healing to occur and prevent recurrence of symptoms. The number of days off work will depend on each worker's individual response and should agree with the recommendations of the treating physician; however, this typically involves from 6 to 12 weeks recovery after carpal tunnel surgery.
(4) Return to Work. A physical evaluation of the worker after time away from work, to assess work capabilities, should be performed to ensure appropriate job placement.
When an employee returns to work after time off, after an operation, or to rest an inflamed tendon, ligament, or nerve, there must be a reconditioning of the healing muscle-tendon groups. (See the guidance on "Conditioning Period Followup" in 111. C. 1.b.) Consideration should be given to permanently reassigning the worker to an available job with the lowest risk of developing CTDs.
(5) The effectiveness of Vitamin B-6 and hot wax for treatment of CTDs has not been established. The use of Vitamin B-6, anti-inflammatory medications such as aspirin, hot wax, constrictive wrist wraps, and a variety of exercise programs have been advocated as effective methods for preventing work-related musculoskeletal disorders of the upper extremity. NIOSH and OSHA, however, are unaware of any scientifically valid research that establishes the effectiveness of these interventions. Exercises that involve stressful motions or an extreme range of motions or that reduce rest periods may actually be harmful.
(6) Every attempt to evaluate, treat, or follow up a worker with complaints of a CTD should be documented by the servicing health care provider in the individual employee medical record.
- Screening Assessment. Upon the employee's presentation of symptoms, the health care provider's screening assessment should include obtaining a history from the worker to identify the location, duration and onset of pain, discomfort, swelling, tingling and/or numbness, and associated aggravating factors. A brief, non-invasive screening examination for the evaluation of CTDs consists of inspection, palpation, range of motion testing, and various applicable maneuvers. (See Barbara Silverstein, Evaluation of Upper Extremity and Low Back, Selected Bibliography.)
- Recordkeeping-OSHA Recordkeeping Forms
The Occupational Safety and Health Act and recordkeeping regulations in Title 29 Code of Federal Regulations (CFR) 1904 provide specific recording requirements that comprise the framework of the occupational safety and health recording system. The Bureau of Labor Statistics (BLS) has issued guidelines that provide official Agency interpretations concerning the recordkeeping and reporting of occupational injuries and illnesses. These guidelines, U . S. Department of Labor, BLS: Recordkeeping Guidelines for Occupational Injuries and Illnesses, September 1986 (or later editions as published), provide supplemental instructions for the OSHA recordkeeping forms (OSHA Forms 200, 101, and 200-S) and should be available in every plant health care facility. Since health care providers often provide information for OSHA logs, they should be aware of recordkeeping requirements and participate in fulfilling them.- Occupational Illnesses. Under the OSH Act, all work-related illnesses must be recorded on the OSHA- 200 form, even if the condition is in an early stage of development. Diagnosis of these conditions may be made by a physician, registered nurse, or by a person who, by training or experience, is capable of making such a determination. If the condition is "diagnosed or recognized" as work-related, the case must be entered on the OSHA-200 form within 6 workdays after detection.
Most conditions classified as CTDs will be recorded on the OSHA-200 form as an occupational illness under the "7f" column, which are "disorders associated with repeated trauma." These are disorders caused, aggravated, or precipitated by repeated motion, vibration, or pressure.
In order to be recordable, the following criteria must be met:
(1) The illnesses must be work related. This means that exposure at work either caused or contributed to the onset of symptoms or aggravated existing symptoms to the point that they meet OSHA recordability criteria. Simply stated, unless the illness was caused solely by a non-work-related event or exposure off premises, the case is presumed to be work related. Examples of work tasks or working conditions that are likely to elicit a work-related CTD are as follows:- Repetitive and/or prolonged physical activities.
- Forceful exertions, usually with the hands (including tools requiring pinching or gripping).
- Awkward postures of the upper body, including reaching above the shoulders or behind the back, and angulation of the wrists to perform tasks.
- Localized contact areas between the work or workstation and the worker's body; i.e., contact with surfaces or edges.
- Excessive vibration from power tools.
- Cold temperatures.
A CTD must exist. There must be either physical findings, OR subjective symptoms and resulting action. Namely, there must be either:- At least one physical finding (e.g., positive Tinel's, Phalen's, or Finkelstein's test; or swelling, redness, or deformity; or loss of motion); OR
- At least one subjective symptom (e.g., pain, numbness, tingling, aching, stiffness, or burning), and at least one of the following:
(i) medical treatment (including self-administered treatment when made available to employees by their employer), (ii) lost workdays (includes restricted work activity); or (iii) transfer/rotation to another job.
(3) If the above criteria are met, then a CTD illness exists that must be recorded on the OSHA-200 form.
EXAMPLE. A production line employee reports to the health unit with complaints of pain and numbness in the hand and wrist. The employee is given aspirin and, after a followup visit with no change in symptoms, is reassigned to a restricted duty job. Even though there are no positive physical signs, the case is recordable because work activity was restricted. - Occupational Injuries. Injuries are caused by instantaneous events in the work environment. To keep recordkeeping determinations as simple and equitable s possible, back cases are classified as injuries even though some back conditions may be triggered by an instantaneous event and others develop as a result of repeated trauma. (See BLS Recordkeeping Guidelines, Selected Bibliography. )
Any occupational injury involving medical treatment, loss of consciousness, restriction of work or motion, or transfer to another job is to be recorded on the OSHA-200 form. Refer to the BLS guidelines for a definition of "medical treatment." - Other Considerations. (1) A case is considered to be complete once there is complete resolution of the signs and symptoms. After resolution of the problem, if signs or symptoms recur, a new case is established and thus must be recorded on the OSHA-200 form as such. Furthermore, failure of the worker to return for care after 30 days indicates symptom resolution. Any visit to a health care provider for similar complaints after the 30-day interval implies reinjury or reexposure to a workplace hazard and would represent a new case.
(2) It is essential that required data, including job identification, be consistently, fully, and accurately recorded on the OSHA-200 form. "Job identification" will include the appropriate job title for "Occupation" and the appropriate organizational unit for "Department" on the OSHA-200.
(3) OSHA recognizes that when an effective ergonomics program is implemented and occupational illnesses and injuries are recorded properly on the OSHA-200 form, the plant's total annual number of CTDs may increase. When engineering and administrative controls are put into place, however, these numbers should gradually decrease.
(4) Health care providers and others should contact the BLS Regional Office or participating State agency serving their area with questions regarding OSHA recordkeeping. Refer to the BLS guidelines (or the list at the end of these guidelines) for addresses and telephone numbers of Regional Offices.
- Occupational Illnesses. Under the OSH Act, all work-related illnesses must be recorded on the OSHA- 200 form, even if the condition is in an early stage of development. Diagnosis of these conditions may be made by a physician, registered nurse, or by a person who, by training or experience, is capable of making such a determination. If the condition is "diagnosed or recognized" as work-related, the case must be entered on the OSHA-200 form within 6 workdays after detection.
- Monitor Trends
- Health care providers should periodically (e .g., quarterly) review health care facility sign-in logs, OSHA-200 forms, and individual employee medical records to monitor trends for CTDs in the plant. This ongoing analysis should be made in addition to the "symptoms survey" (described previously in this Section) to monitor trends continuously and to substantiate the information obtained in the annual symptoms survey. The analysis should be done by department, job title, work area, etc. (See also Section 111. A., " Worksite Analysis Program.")
- The information gathered from the annual symptoms survey will help to identify areas or jobs where potential CTD problems exist. This information may be shared with anyone in the plant, since employees' personal identifiers are not solicited. The analysis of medical records (e.g., sign-in logs and individual employee medical records) may reveal areas or jobs of concern, but it may also identify individual workers who require further followup. The information gathered while analyzing medical records will be of a confidential nature; thus care must be exercised to protect the individual employee's privacy.
- The information gained from the CTD trend analysis and symptoms survey will help determine the effectiveness of the various programs initiated to decrease CTDs in the plant.
Exhibit 1
Symptoms Survey: Ergonomics Program
Symptoms Survey: Ergonomics Program
Date ____/____/____
Plant Dept Job # Job Name
years months
Shift Supervisor Hours worked/week Time on THIS job
Other jobs you have done in the last year (for more than 2 weeks)
months weeks
Job # Job Name Time on THIS job
months weeks
Dept Job # Job Name Time on THIS job
(If more than 2 jobs, include those you worked on the most)
Have you had any pain or discomfort during the last year?
1)Yes 2)No (If NO, stop here)
If YES, carefully shade in the area of the drawing which bothers you the most.
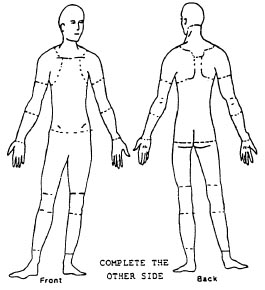
(Complete a separate page for each area that bothers you)
Check Area: Neck Shoulder Elbow/Forearm Hand/Wrist Fingers
Upper Back Low Back Thigh/Knee Low Leg Ankle/Foot
1. Please put a check by the word(s) that best describe your problem
1) Aching 5) Numbness(asleep) 9) Tingling
2) Burning 6) Pain 10) Weakness
3) Cramping 7) Swelling 11) Other
4) Loss of Color 8) Stiffness
2. When did you first notice the problem (month) (year)
3. How long does each episode last? (Mark an X along the line)
1 hour 1 day 1 week 1 month 6 months
/ / / /
4. How many separate episodes have you had in the last year?
5. What do you think caused the problem?
6. Have you had this problem in the last 7 days? 1)Yes 2)No
7. How would you rate this problem (mark an X on the line)
Now
None Unbearable
When it was the WORST
None Unbearable
8. Have you had medical treatment for this problem? 1)Yes 2)No
8a. If NO, why not
8b. If YES, where did you receive treatment?
1. Company Medical Times in past year
2. Personal doctor Times in past year
3. Other Times in past year
8c. If YES, did the treatment help? 1)Yes 2)No
9. How much time have you lost in the last year
because of this problem? days
10.How many days in the last year were you on restricted
or light duty because of this problem? days
11.Please comment on what you think would improve your symptoms.
Exhibit 2
Screening Tests
Positive Tinel's sign: Gentle tapping over the median nerve at the wrist
resulting in pain, tingling, or numbness in the
median nerve distribution.
Positive Finkelstein's test: Ulnar deviation of the hand with the thumb flexed
against the palm and the finger flexed over the thumb.
Severe pain results at the radial styloid due to
stretching of the abductor pollicus longus and extensor
pollicus brevis.
Positive Phalen's test: Unforced, complete flexion of the wrist for 60 seconds
resulting in pain, numbness, or tingling in the median
nerve distribution
Exhibit 3
Upper Extremity (UE) Cumulative Trauma
Disorders (CTDs) Algorithm
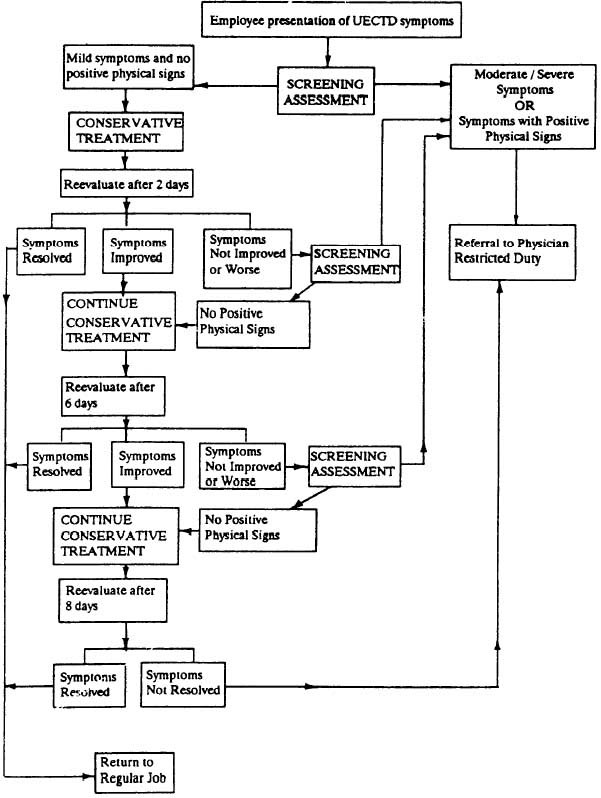
Selected Bibliography for Ergonomics Program Management in the Meatpacking Industry
Primary Sources cited in the Guidelines:
Putz-Anderson, Vern, Ed. Cumulative Trauma Disorders: A Manual for Musculoskeletal Diseases of the Upper Limbs. London: Taylor and Francis, 1988. 151 Pp.
Silverstein, Barbara A. and Fine, Lawrence J. Evaluation of Upper Extremity and Low Back Cumulative Trauma Disorders -- A Screening Manual. Ann Arbor, Michigan: University of Michigan. School of Public Health , Occupational Health Program , 1984. 43 Pp.
U.S. Department of Health and Human Services. Work Practices Guide for Manual Lifting. Public Health Service. Centers for Disease Control. National Institute for Occupational Safety and Health. DHHS(NI0SH) Pub. No. 81-122. Cincinnati, Ohio. 1981. 183 Pp:
Criteria for a Recommended Standard on Occupational Exposure to Hand-Arm Vibration. National Institute for Occupational Safety and Health. Publication No. 89-106. Cincinnati: NIOSH, 1989. 127 Pp.
U.S. Department of Labor. Bureau of Labor Statistics. Recordkeeping Guidelines for Occupational Injuries and Illnesses. OMB . No. 1220-0029. Washington, D.C. : Government Printing Office, September 1986 (or later editions as published). 84 Pp.
Additional Sources
American Meat Institute. Management Strategies for Preventing Strains and Sprains: A Guide to Practical Ergonomics. Washington D . C. 1988. 27 Pp.
Armstrong, T.J. An Ergonomics Guide to Carpal Tunnel Syndrome. Akron, Ohio: American Industrial Hygiene Association, 1983.
Carlsson, A. "Hand Injuries in Sweden in 1980" journal of of Occupational Accidents. Vol. 6, No. 1-3, pp. 155-165, 1984.
Chaffin, D.B. "Ergonomics Guide for the Assessment of Human Static Strength." American Industrial Hygiene Association Journal. 36. 505-511, 1975.
Chaffin, D.B. and G.B.J. Andersson. Occupational Biomechanics. New York: John Wiley, 1984.
Cochran, D.J. An Investigation of Safe Handle Design. U.S. Department of Health and Human Services. National Institute for Occupational Safety and Health. Grant No 1 -Rol-OH-0 1 134-01. Cincinnati, 1982. 215 Pp.
Cochran, D.J., and Riley, M.W. "An Evaluation of Knife Handle Guarding," Human Factors, Vol , 28, No. 3, pp. 295-301, 1986.
Cranz, A., et al. "The Role and Organization of Industrial Medicine in Slaughter Houses and Meat Markets." Archives des Maladies Professionnelles de Medicine de Travail et de Securite Sociale. Vol. 31, NO. 9, pp. 485-490, 1970.
Eastman Kodak Company, Ergonomics Group. Ergonomic Design for People at Work. New York: Van Nostrand Reinhoid Co., Vol. 2, 1986.
Eastman Kodak Company, Human Factors Section. Ergonomic Design for People at Work. Belmont, California:
Lifetime Learning Publications, Vol. 1, i983.
Falck, B., and Aarnio, P. "Left-Sided Carpal Tunnel Syndrome in Butchers". Scandinavian Journal of work, Environment & Health, Vol. 9, NO. 3, 1983.
Finkel, M.L. "The Effects of Repeated Mechanical Trauma in the Meat Industry." American Journal of Industrial Medicine. Vol. 8, No. 4-5, pp. 375-379, 1985.
Fraser. T.M. Ergonomic Principles in the Design of Hand Tools. (Occupational Safety and Health Series No. 44). Geneva, Switzerland: International Labour Office, 1980.
Hagberg, M. , and Wegman, D.H. "Prevalence Rates and Odds Ratios of Shoulder-Neck Diseases in Different Occupational Groups." British Journal of Industrial Medicine. Vol. 44, No. 9; pp. 602-610, 1987.
Jensen, R.C., et al. "Motion-Related Wrist Disorders Traced to Industries, Occupational Groups." Monthly Labor Review, Vol. 106, pp 13-16, 1983
Kropf, D.H., and Breidenstein, B.C. Beef Operations in the Meat Industry. Report No. SR-537. Washington, D.C., American Meat Institute, 1975. 141 Pp.
Kvalseth, T.Q. Ergonomics of Workstation Design. London: Butterworths. 1983.
Magnusson, M., et al. "An Ergonomic Study of Work Methods and Physical Disorders Among Professional Butchers." Applied Ergonomics. Vol. 18, No. 1, pp. 43-50, 1987.
Magnusson, M., and Ortengren, R. "Investigation of Optimal Table Height and Surface Angle in Meatcutting." Applied Ergonomics. Vol. 18, No. 2, pp. 146-152, pp. 1987.
National Safety Council. Meat Industry Safety Guidelines. Chicago, Illinois, 2nd Edition, 1978.
Nielsen, R. "Clothing and Thermal Environments." Applied Ergonomics. Vol. 17, No. 1, pp. 47-57. 1986.
Pezaro, A. Critical Review Analysis for Injury Related Research in the Meatpacking Industry (SIC 2011). NIOSH 00144940. U.S. Department of Health and Human Services. National Institute for Occupational Safety and Health. Cincinnati, 1984.
Polakoff, P.L., and Vandervort, R. Health Hazard Evaluation. Report No. HHE-7 1-29-89. Sioux Falls, South Dakota: John Morrell Company, 1973.
Riley, M. W., and Cochran, D.J. Proceedings of the Symposium on Occupational Safety Research and Education. NIOSH Publication No. 82-103. U.S. Department of Health and Human Services. National Institute for Occupational Safety and Health. Cincinnati, January 1981, pp. 67-74.
Roto, P., and Kivi, P. "Prevalence of Epicondylitis and Tenosynovitis Among Meat Cutters." Scandinavian Journal of Work, Environment & Health. Vol. 10, No. 3, 1984.
Salvendy , G., and Smith, M. J. Machine Pacing and Occupational Stress. London: Taylor & Francis, Ltd., 1981.
Streib, E. W., and Sun, S.F. "Distal Ulnar Neuropathy in Meat Packers: An Occupationa Disease." Journal of Occupational Medicine. Vol. 26, No. 11, pp. 842-843, 1984.
Tichauer, E. R. and Gage, H. "Ergonomic Principles Basic to Hand Tool Design." American Industrial Hygiene Association Jouml. Vol. 38, pp. 622-634, 1977.
U.S. Department of Health and Human Services. National Institute for Occupational Safety and Health. Occupational Hazards in Animal Rendering Processes. Cincinnati, 1981.
U. S. Department of Labor. Occupational Safety and Health Administration. Safety and Health Guide for the Meatpacking Industry. OSHA Publication No. 3 108. Washington, D.C., 1988. 12 Pp.
Viikari, J.E. "Neck and Upper Limb Disorders Among Slaughterhouse Workers. An Epidemiologic and Clinical Study." Scandinavian Journal of Work, Environment & Health. Vol 9, No. 3, pp. 283-290, 1983.
Glossary
A wide variety of terms are currently used by employers, occupational safety and health professionals, and others in describing ergonomic 2rograms. The following definitions are provided to clarify the terms used by OSHA in the ergonomic program management guidelines:
"Cumulative trauma disorders (CTDs)" is the term used in these guidelines for health disorders arising from repeated biomechanical stress due to ergonomic hazards. Other terms that have been used for such disorders include "repetitive motion injury," "occupational overuse syndrome," and "repetitive strain injury."
CTDs are a class of musculoskeletal disorders involving damage to the tendons, tendon sheaths, synovial lubrication of the tendon sheaths, and the related bones, muscles, and nerves of the hands, wrists, elbows, shoulders, neck and back. The more frequently occurring occupationally induced disorders in this class include carpal tunnel syndrome, epicondylitis (tennis elbow), tendonitis, tenosynovitis , synovitis, stenosing tenosynovitis of the finger, DeQuervain's Disease, and low back pain.
"Ergonomic hazards" refer to workplace conditions that pose a biomechanical stress to the worker. Such hazardous workplace conditions include, but are not limited to, faulty work station layout, improper work methods, improper tools, excessive tool vibration, and job design problems that include aspects of work flow, line speed, posture and force required, work/rest regimens, and repetition rate. They are also referred to as "stressors."
"Ergonomic risk factors" are conditions of a job, process, or operation that contribute to the risk of developing CTDs. Examples include repetitiveness of activity, force required, and awkwardness of posture; for further discussion, see Section 111. A. Risk factors are regarded as synergistic elements of ergonomic hazards which must be considered in light of their combined effect in inducing CTDs. Jobs, operations, or work stations that have multiple risk factors will have a higher probability of causing CTDs, depending on the relative degree of severity of each factor.
"Ergonomics team" refers to those responsible for identifying and correcting ergonomic hazards in the workplace, including ergonomic professionals or other qualified persons, health care providers, engineers and other support personnel, plant safety and health personnel, managers, supervisors, and employees.
"Ergonomist" or "ergonomics professional" means a person who possesses a recognized degree or professional credentials in ergonomics or a closely allied field (such as human factors engineering) and who has demonstrated, through knowledge and experience, the ability to identify and recommend effective means of correction for ergonomic hazards in the workplace.
"Health care provider" is a physician who specializes in occupational medicine, or a registered nurse specializing in occupational health, or other health personnel (such as emergency medical technicians) working under the supervision of a physician or registered nurse. Health care providers will have the training outlined in Appendix B, "Medical Management Program."
"Qualified person" means one who has training and experience sufficient to identify ergonomic hazards in the workplace and recommend an effective means of correction. An example would be a plant engineer fully trained in ergonomics.
A "systems approach" to safety and health management means a comprehensive program by the employer which addresses workplace processes, operations, and conditions as interdependent systems in order to identify and to eliminate or reduce all types of hazards to employees. Thus, complex ergonomic problems may require a combination of solutions.
Ergonomics Program Management Guidelines for Meatpacking Plants -- Questions and Answers
GENERAL/SCOPE
1. Q: Do the guidelines apply to just red meat plants? What about sausage processors, or fish and poultry?
A: The guidelines are being sent to every establishment in Standard Industrial Classification (SIC) code 2011, "Meat Packing Plants -large and small- which covers red meat processing establishments that include slaughtering. They are specifically intended to cover facilities in that SIC code, because OSHA's special emphasis program (SEP) will be confined to SIC 2011.
However, OSHA believes that all of the general guidance, and much of the specific guidance, can and should be applied to establishments in other industries, especially fish and poultry processing. OSHA encourages employers in other industries to use the guidelines in developing and implementing their own ergonomics programs.
2. Q: I'm a small employer in the meatpacking industry. How do this program and the guidelines affect me?
A: As noted above, the guidelines are being sent to every meatpacking facility, large and small. So far, the ergonomic problems that OSHA and other experts have identified in this industry have been concentrated in the larger plants. This may be due to their production operations and the amounts of repetitive motion expected of workers in these plants. Accordingly, the enforcement part of this program will be directed, at first, to larger meatpacking employers.
However, small employers in the industry should also take a careful look at their workplaces to determine if they have similar problems; and if so, they should take appropriate actions to correct them. The guidelines are provided to help employers do this. The OSHA consultation program can also be of assistance (see questions 30 and 33). OSHA hopes to work with employers of all sizes over the course of this program to find out what specific problems exist, and what the best ways of dealing with them are.
3. Q: Why don't the guidelines provide examples of how small meatpackers can adapt the program elements to their own needs and resources? Will OSHA provide more guidance later?
A: The guidelines were developed primarily with a view to the larger meatpacking employers where the greatest ergonomic problems are known to exist-and where most of the employees in the industry work. OSHA believes, however, that the guidelines can and should be adapted to the circumstances of meatpacking employers of all sizes. Sample compliance plans were not included because of the wide variety of plant sizes, products, operations, and conditions in the meatpacking industry. It would not be possible-and perhaps misleading-for OSHA to make such specific recommendations at this stage of the program, beyond that already given in the guidelines.
An important part of this program will be the learning process-for OSHA, employers, and employees about how to identify and solve ergonomic problems. OSHA will work cooperatively with small employers to try out techniques for preventing and correcting ergonomic problems, so that successful methods can be passed on to other employers. OSHA will be distributing a new publication called "ErgoFacts" to highlight successful means of solving ergonomic problems. In addition, if experience warrants, OSHA may publish a revised version of the guidelines at a later point in the program.
4. Q: The guidelines are all about ergonomic hazards in meatpacking. Are the other safety and health hazards in meatpacking (e.g., cuts, slips & falls) under control? Is OSHA still going to be enforcing on those?
A: The other hazards still remain, which is a major reason why SIC 2011 is consistently listed as a high hazard industry. OSHA will continue to enforce compliance with standards which relate to those hazards, and employers must continue with safety and health programs to control them. OSHA will also continue to accord the same priority for conducting safety and health inspections in both large and small meatpacking plants as before.
5. Q: What about workers with off-the-job activities that contribute to CTDs?
A: The guidelines are intended to be applied to workplace conditions over which the employer exercises control. Both OSHA and NIOSH acknowledge that, at present, there is no scientifically validated test or other means to determine which individuals are at risk of developing CTDs.
CTDs arise from repeated biomechanical stress to a particular part of the body. The length of time employees spend on the job indicates that risk from ergonomic stressors in the workplace is proportionately greater, and therefore must be controlled to the extent feasible.
In terms of recordability for OSHA recordkeeping regulations, BLS guidelines state that, unless a CTD illness was caused solely by a non-work-related event or exposure off-premises, it is presumed to be work related.
ENFORCEMENT
6. Q: Is this a new regulation? Will I be cited for not following the guidelines?
A: This is not a new standard or regulation. We expect employers to implement an effective ergonomics program which contains the major program elements described in the guidelines. OSHA's field inspection staff have been instructed that failure to implement the guidelines is not in itself a violation of the General Duty Clause of the OSH Act. The guidelines provide information on the steps employers should take (1) to determine if they have ergonomic-related problems in their workplaces, (2) to identify the nature and location of those problems, and (3) to implement measures to reduce to eliminate them.
7. Q: How is OSHA going to enforce ergonomics?
A: As in the past, employers will be cited, where appropriate, for violations of Section 5(a)(l) of the OSH Act - the General Duty Clause - for employee exposure to ergonomic hazards. Employers who develop effective programs and implement them fully in their workplaces will have taken appropriate steps to substantially reduce or eliminate ergonomic hazards that could be subject to citation. The guidelines are intended to help meatpacking employers understand what OSHA considers when it inspects a workplace.
8. Q: When can I expect an OSHA ergonomics inspection? Will there be some "lead time" to allow employers to begin implementing the guidelines before inspections start?
A: The initial enforcement emphasis of the SEP will be on a limited number of comprehensive inspections- covering safety, health , and ergonomics-in larger meatpacking establishments. These will begin in the latter part of 1990. The inspections in this program will be carefully planned and targeted, but otherwise will be similar to the major ergonomics inspections OSHA has conducted in several meatpacking plants over the past few years in response to specific complaints. The comprehensive inspections will cover all aspects of workplace safety and health, including ergonomics, and recordkeeping.
For the smaller establishments, OSHA will probably continue to inspect workplaces in SIC 2011 with about the same frequency as it currently is doing, in response to complaints and fatalities and as part of the general schedule programming of high hazard workplaces. There are usually a few hundred of these each year, because meatpacking is a hazardous industry.
Whex OSHA looks at ergonomics in smaller establishments, it will simply be to determine if the employer has a problem, and if so, if steps (such as those described in the guidelines) are being taken to deal with it. Citations will not be issued for failure to follow the specific guidelines. If an employer has a serious problem that he or she is not addressing, however, a citation for violation of Section 5(a)(l) may be issued.
COMPLIANCE
9. Q: What does it mean to adapt the program elements to the size and circumstances of the workplace?
A: The guidelines are not intended to be "one size fits all." OSHA regards each of the program elements-worksi te analysis, hazard prevention and control, training and education, and medical management- as essential to a comprehensive program. Every meatpacker's ergonomics program should include all of them. But the manner and extent to which they are implemented will vary according to the size of the plant and its workforce, its operations, its product, its current safety and health program, and the extent of any ergonomic problems. OSHA does not expect small employers to have exactly the same problems - or solutions - as larger employers. The aim of the guidelines is for all meatpacking employers to set about identifying and correcting ergonomic hazards in the same systematic way.
The first step for all employers-large and small-should be to assess the extent of any problems they may have related to ergonomic hazards. They should use a systematic method of worksite analysis, such as that recommended in the guidelines, to do this. They should then take whatever measures are appropriate including those set forth in the guidelines-to address the problems found, if any. If, after conducting this systematic analysis, the employer determines that there is no problem, then further implementation of the program would be limited to monitoring workplace conditions for changes and responding accordingly.
As this effort continues, OSHA hopes to work with employers of all sizes in sharing our acquired experience in implementing effective ergonomic programs and finding solutions to common problems.
10. Q: What are the "program elements" I am supposed to be adapting? The guidelines have a number of sections and subsections-do I have to follow all of them? Are some more important than the rest?
A: As described at the beginning of Section 11, there are four major program elements that OSHA regards as essential to a good ergonomics program: (1) worksite analysis, (2) hazard prevention and control, (3) medical management. and (4) training and education.
Although they are all important and should be included in the employer's program, worksite analysis should get first attention. That is, the employer should first analyze the workplace to find out what ergonomic problems now exist, and begin determining how to correct them.
11. Q: The "systematic method" the guidelines describe for worksite analysis seems very technical and complicated. Is all of this necessary for a small plant?
A: The analysis should be systematic-step-by-step- in order to prevent it from becoming more complicated or extensive than it needs to be. The first step is looking at the injury and illness records every employer should keep to determine if employees are experiencing cumulative trauma disorders-or any related problems that may have been entered on the OSHA-200 log-and to see which jobs are presenting the problems. In a small establishment it may be relatively simple to find out where problems, if any, exist.
For smaller employers, OSHA does not believe a complicated effort should be necessary. Look at your injury/illness records. review any workers' compensation claims, look at the work as it is being done and ask questions of employees to see if there are ergonomic problems. Identify the jobs that appear to have the problems, and determine if those jobs involve ergonomic risk factors. You should then take whatever measures are appropriate-including those set forth in the guidelines-to address the problems found, if any. If no problems exist, you should keep on with your current efforts to maintain a safe and healthful workplace.
12. Do I have to get a consultant to help perform surveys and analyze jobs? Is videotaping required?
Once the employer has determined which jobs are showing problems, those jobs then should receive a more rigorous analysis to pinpoint the "risk factors" that are causing the problems, such as posture, repetition, and force. This is where a consultant, or advice from an OSHA office, can be most helpful. However, a great deal can be accomplished by using common sense and discussing the job with the employees who do it.
Videotaping is one method that can be very useful in analyzing jobs; many consultants use it because it helps in taking a close look at work operations off-site. It is not required, however, and is recommended only for those jobs that have already been identified as having problems. Its value lies in being able to look at work tasks in slow motion and to break down their elements. When videotaping is done it should only require a few minutes for each job being analyzed enough to capture the full cycle of the work task.
13. Q: Do I need a special written program just for ergonomics?
A: OSHA is recommending that every employer in SIC 2011 implement a comprehensive program to address ergonomic hazards in the workplace. Although this should be done as part of a sound overall safety and health program, OSHA believes that it is essential that there should be either a separate written program for ergonomics, or a separate section of the employer's overall written safety and health program. OSHA has found that a written program is an invaluable management tool to ensure consistency in the program's implementation, to establish definite goals and timetables. and to assign responsibilities.
14. Q: Do OSHA guidelines require me to make expensive workstation design changes and go out and buy new equipment?
A: Any changes in workstations or equipment should be determined by the employer's ergonomics team to be appropriate for the specific conditions in the plant. Although changes in workstation design and equipment used are the preferred means of hazard prevention and control, as discussed in the guidelines, they are not the only means. OSHA's guidelines recommend that employers first identify the ergonomic problems in their workplaces, analyze those problems to determine appropriate means of correcting them, and implement the corrective measures. Also important among possible control measures are improvements in the design of work operations or jobs, and in the work practices employees use.
It has been OSHA's experience that many changes to equipment and workstation design that are effective in correcting ergonomic hazards are also not costly and relatively simple, involving comparatively little in modifications to existing conditions. Moreover, the most effective solution is not necessarily the most expensive. Purchases should therefore be made carefully, after thorough analysis of the circumstances.
15. Q: Does this require slowing down the line?
A . this is one of a wide variety of control measures that can be implemented to address specific, identified problems. Modifying line speed is one means of work method design that may be appropriate after a systematic worksite analysis has been conducted to determine the nature of existing problems. The guidelines (Sections 11. B. and 111. B.) provide a number of examples of engineering, work practice, and administrative controls.
16. Q: What is a "break-in period"?
A: Most jobs in the meat industry will require conditioning or break-in periods, which may last several weeks, for new and transferred employees to condition their muscle-tendon groups prior to working at full capacity. Use of a break-in period is recommended by the American Meat Institute in its "Ergonomics and Safety Guidelines" (1989). It is that time before an employee is expected to "pull full count-for example, when the employee gradually works up from performing the assigned task on every 10th carcass coming down the line to performing it on every second or third. The length of the break-in period varies with the job; a typical time is about a month.
17. Q: Am I supposed to have a special training line just for workers in the break-in period? Do I have to slow down the line for this period every time a new employee is hired?
A: A special training line or area is highly recommended, based on OSHA's experience in this industry. It is especially needed where production lines move at high speeds, or in any meatpacking workplace where there is a considerably higher rate of injury to new workers than to experienced ones. A special training line is not necessary, however, to accommodate a break-in period when employees are gradually working up to full capacity. While break-in procedures may involve adjusting numbers of employees on the line, they do not necessarily entail slowing the line.
18. Q: What does OSHA mean by "providing sufficient numbers of standby/relief personnel" as an administrative control?
A: One of the administrative control methods suggested by the guidelines is providing sufficient numbers of standby or relief personnel to compensate for foreseeable upset conditions on the line, such as a decrease in the number of workers normally on the line due to absences or other reasons. This would help to ensure that remaining workers are not overburdened by having to make up for the upset by increasing their output, thereby increasing ergonomic stress.
19. Q: When the guidelines refer to a specific knife sharpening program, does this mean we must switch from individual sharpening to centralized sharpening?
A: The guidelines recommend having a specific knife sharpening program-clearly established procedures to ensure that workers have adequate opportunity to sharpen their knives or obtain a sharpened knife-so that sharp knives are always readily available for workers who need them. Using knives that are not properly sharpened causes the worker to use greater force, thus increasing ergonomic stress. Employers may use either individual or centralized sharpening, as appropriate for conditions in their plant.
20. Q: We just buy tools, not design them. How are we supposed to control tool design?
A: OSHA realizes that meatpacking employers, in most cases, do not design the tools they use. However, employers should select and purchase well-designed tools to minimize ergonomic stressors and replace poorly designed ones. They can also exercise their influence as the consumers of such tools to ask for improved designs from the tool manufacturers.
21. Q: What does job rotation mean? A worker does one job in the morning and another in the afternoon? Switching jobs every week-or month-or three months?
A: Job rotation can mean that a worker performs two or more different tasks in different parts of the day. (For example, switching between task "A" and task "B" at 2-hour or 4-hour intervals.) The important consideration is to ensure that the different tasks do not present the same ergonomic stressors to the same parts of the body (muscle-tendon groups). There is no single work-rest regimen that OSHA recommends; it must be determined by the nature of the task.
22. Q: The guidelines state that "if job rotation is utilized, the job analyses must be reviewed by a qualified person..." What is a "qualified person"?
A: As discussed in the glossary of the guidelines, a "qualified person" is one who has thorough training and experience sufficient to identify ergonomic hazards in the workplace and recommend an effective means of correction; for example, a plant engineer fully trained in ergonomics-not necessarily an ergonomist. For job rotation, the important consideration is that the different jobs between which employees rotate should use different muscle-tendon groups, to minimize ergonomic stress. In analyzing jobs for job rotation, the qualified person must have sufficient expertise to identify the ergonomic stressors each job presents and which muscles and tendons are used.
23. Q: Based on my experience and records, I don't believe my plant has a problem. Do I have to implement a program?
A: The first step in implementing the program is a systematic worksite analysis, including a thorough review of injury/illness data and workstation screening surveys. After performing these, the employer will be able to determine the extent of the ergonomic hazards and identified cumulative trauma disorders (CTDs) in the workplace. These findings will indicate any further steps the employer should take. If, after conducting this systematic analysis, the employer determines that there is no problem, then further implementation of the program would be limited to monitoring workplace conditions for changes and responding accordingly.
MEDICAL MANAGEMENT
24. Q: When the guidelines refer to a health care provider being part of the ergonomic team, does this mean I am required to have a full-time medical expert to oversee our medical management program?
A: The guidelines recommend that the medical management program should be designed by and operated under the supervision of an occupational medicine physician (a medical doctor trained and experienced in the prevention and treatment of workplace injuries and illnesses) or an occupational health nurse (a registered nurse trained and experienced in the prevention and treatment of workplace injuries and illnesses). All other health care providers or medical personnel who may be involved in the employer's medical management program should be answerable to such a medical professional.
OSHA would like every employer to have the best medical program possible. Obviously, however, an employer's program for providing medical care for employees will vary according to the needs, circumstances, and resources of the plant. Smaller employers which do not employ a physician or nurse - or perhaps do not even have a medical facility on the premises may, however, have an established relationship with a physician or health care facility to which injured or ill employees routinely go. They might also engage the services of an occupational health nurse on a part-time or consultative basis to oversee their program. OSHA strongly recommends that these health care providers be made familiar with the types of hazards to be found in the employer's workplace. In addition, the health care providers should be familiar with the recommendations in the guidelines on medical management programs.
25. Q: Is every plant expected to have a full-time occupational health nurse on duty?
A: The guidelines recommend that "each work shift should have access to health care providers" and that "appropriately trained health care providers should be available at all times." While it would be highly desirable to have a full-time occupational health nurse on duty in every plant, OSHA recognizes that this will not be possible for all employers, particularly small employers. The important consideration is for employees to have access to medical care at appropriate times from health care providers-onsite or off-site-who are familiar with the types of safety and health hazards the employees may encounter in their workplace, including ergonomic hazards.
The employer's health care providers should be familiar with the recommendations in the guidelines on medical management programs. This recommendation applies especially when the employer's ergonomics program requires an extensive or complex medical management effort.
26. Q: How do I find an occupational health nurse?
A: The American Association of Occupational Health Nurses (AAOHN) should be able to recommend qualified nurses, either directly or by referring an employer to its local chapter. The address and telephone number of the National headquarters of AAOHN is:
American Association of Occupational Health Nurses
56 Lenox Pointe
Atlanta, Georgia 30324
Telephone: (404) 262-1162
27. Q: Where do I find an occupational medicine physician?
A: Local branches of the American Medical Association (AMA) should be able to recommend occupational medicine physicians. Information may also be obtained from the American College of Occupational Medicine in Chicago, Illinois [telephone: (708)228-6850. It should be remembered that not all physicians have the training and experience in occupational medicine needed for medical management of a good workplace ergonomics program.
28. Q: Dc paramedics, emergency medical technicians, or qualified first aid individuals qualify as medical experts in the eyes of OSHA's ergonomics guidelines?
A: Paramedics, emergency medical technicians, and qualified first aid individuals would not be regarded as medical experts. They may, however, be among the health care providers involved in the employer's medical management program. Such health personnel should be working under the supervision of a physician or a registered nurse, should have basic training in the recognition and treatment of CTDs, and should be familiar with the recommendations in the guidelines on medical management programs.
29. Q: The medical management guidelines call for putting workers with CTDs on restricted duty jobs. What if there are no such jobs - or not enough? Can such workers be laid off/fired?
A: Removing employees who have actual or potential CTDs from exposure to ergonomic hazards is an essential part of an effective medical management program. Such workers should be placed in light or restricted duty jobs, or in some other status which does not add to their ergonomic risk, in order to allow the affected muscle-tendon group to rest. Implementing administrative measures to protect the pay and employment status of workers who need to be removed from hazardous exposure will help to ensure that workers who are experiencing problems report them and seek treatment promptly.
RESOURCES
30. Q: I am a small meat packing employer. Do I have to hire an ergonomist? Is an ergonomist necessary for a small plant?
A: The guidelines state that several aspects of the program - e.g., conducting the worksite analysis, determining appropriate controls-can only be done by a qualified person, ideally an ergonomist. OSHA therefore strongly recommends engaging the services of an ergonomist or other properly qualified person.
OSHA realizes, however; that it may be difficult for smaller employers to retain an ergonomist. Small employers may wish to act jointly or through an industry association to do so.
OSHA is also reminding all such employers of the availability of the free (OSHA-funded) consultation service in each State, which is independent of the enforcement program. OSHA is also taking steps to ensure that these consultation services can provide expertise in ergonomics, and that they will be available to small and medium size employers-up to 500 employees-in the meat industry (although there may be waiting periods). In addition, OSHA Area and Regional Offices can answer specific questions employers may have.
31. Q: What is OSHA's definition of an ergonomist? Where do I find one?
A: By "ergonomist" we generally mean a professional with a doctoral/graduate degree in ergonomics or a closely allied field-e.g., industrial engineering, human factors engineering, physiology-who has had sufficient training and experience to competently assess and recommend solutions for ergonomic problems of worksites and work operations.
OSHA recognizes that the number of fully qualified ergonomists available to employers is limited. OSHA's Regional and Area Offices and NIOSH should be able to provide lists of recognized, qualified ergonomists. Industry associations may also be able to provide such information.
32. Q: What is the ergonomics team-who should be on it?
A: As defined in the glossary of the guidelines, the "ergonomics team" refers to those responsible for identifying and correcting ergonomic hazards in the workplace. OSHA recommends a team approach to assessing a workplace's problems and implementing solutions, on an ongoing basis, involving appropriate personnel from all levels. The makeup of the team will vary from plant to plant, depending on the establishment's operations and circumstances and the actual people who have responsibility for some aspect of the ergonomic program in the particular workplace. Personnel who might typically be included are the ergonomist or other qualified person, plant safety and health personnel, management, line supervisors, health care providers, and affected employees.
33. Q: How do I get a consultant? How much will it cost me?
A: OSHA's Regional and Area Offices can provide the name and address of the OSHA Consultation Service for each State. A list of the addresses and telephone numbers of these services is also included with the guidelines. There may be a waiting period for the State consultation service to respond to an employer's request.
OSHA offices and industry associations should be able to provide the names of private consultants; we have no estimates as to their cost. Smaller employers may also wish to act jointly or through an industry association (such as the American Meat Institute, the American Association of Meat Processors, or the National Association of Meat Purveyors) to engage consultants.
34. Q: where and how do I get training for this?
A: OSHA provides general instruction in its "Principles of Ergonomics" course at the OSHA Training Institute, which may have openings for private employers and industry groups. The Training Institute will also be offering a special course for the meatpacking emphasis program, beginning in December 1990 and running quarterly thereafter for the next year or two. The first classes will be restricted to OSHA and State compliance officers and State consultants; later sessions may have openings for private employers.
In addition, OSHA Area and Regional Offices can provide speakers and training sessions for employers or employer groups. This may be of particular interest to smaller employers. OSHA offices will also have copies of an "Ergonomics Training Resource List" now being developed by the OSHA Training Institute. A list of OSHA Regional Office addresses and telephone numbers is provided with the guidelines.
Meatpacking employers should also consult with the American Meat Institute (AMI), the National Association of Meat Purveyors, American Association of Meat Processors, Western States Meat Association, and other industry groups for training resources. OSHA is aware that the AMI, in particular, has demonstrated interest in the development of training resources in ergonomics. Moreover, labor groups such as the United Food and Commercial Workers and the AFLCIO can provide help in training, or work cooperatively with employers in supporting academic training resources. The University of Michigan, for example, conducts special programs in ergonomics; the Universities of Nebraska and Oklahoma also have ergonomics programs.
35. Q: Where do I get the books listed in the bibliography?
A: Copies of some of the books in the bibliography- especially the "primary sources"-may be available for researching in OSHA Regional Office libraries (although most OSHA Regional Offices do not lend books out). Other sources are the National Technical Information Service (NTIS), OSHA's Technical Data Center in Washington, DC, NIOSH, and other technical libraries (such as those at universities).
36. Q: Can I/my organization reproduce the guidelines and distribute them?
A: Yes. In fact, OSHA encourages this. As noted near the beginning of the guidelines booklet, source credit for the U.S. Department of Labor is requested, but not required.
OTHER SOURCES OF OSHA ASSISTANCE
Safety and Health Program Management Guidelines
Effective management of worker safety and health protection is a decisive factor in reducing the extent and severity of work-related injuries and illnesses and their related costs. To assist employers and employees in developing effective safety and health programs, OSHA published recommended Safety and Health Program Management Guidelines (January 26, 1 989,54 FR: 3908-39 16). These voluntary guidelines apply to all places of employment covered by OSHA. The guidelines identify four general elements that are critical to the development of a successful safety and health management program:
- management commitment and employee involvement;
- worksite analysis
- hazard prevention and control; and
- safety and health training
The guidelines recommend specific actions, under each of these general elements, to achieve an effective safety and health program.
State Programs
The OSH Act encourages states to develop and operate their own job safety and health plans. OSHA approves and monitors these plans. There are currently 25 state plan states: 23 of these states administer plans covering both private and public (state and local government) employment; and the other 2 states, Connecticut and New York, cover the public sector only.
The 25 states and territories with their own OSHA approved occupational safety and health plans must adopt standards identical to, or at least as effective as, the federal standards. Until a state standard is promulgated, OSHA will provide interim enforcement assistance. as appropriate, in these states. A listing of states with approved plans appears at the end of this booklet.
Consultation Services
Consultation assistance is available on request to employers who want help in establishing and maintaining a safe and healthful workplace. Largely funded by OSHA, the service is provided at no cost to the employer. Primarily developed for smaller employers with more hazardous operations, the consultation service is delivered by state government agencies or universities employing professional safety and/or health consultants. Comprehensive assistance includes an appraisal of all mechanical, physical work practices, and environmental hazards of the workplace and all aspects of the employer's present job safety and health program. No penalties are proposed or citations issued for hazards identified by the consultant.
For more information concerning consultation assistance, see the list of consultation projects listed at the end of this publication.
Voluntary Protection Programs (VPP)
Voluntary protection programs and onsite consultation services, when coupled with an effective enforcement program, expand worker protection to help meet the goals of the OSH Act. The three VPPs-Star, Merit, and Demonstration- are designed to recognize outstanding achievement by companies that have successfully incorporated safety and health programs into their total management system. They motivate others to achieve excellent safety and health results in the same outstanding way as they establish a cooperative relationship between employers, employees, and OSHA.
For additional information on VPPs and how to apply, contact the OSHA national, regional, or area offices listed at the end of this publication.
Training and Education
OSHA's area offices offer a variety of informational services, such as publications, audiovisual aids, technical advice, and speakers for special engagements. OSHA's Training Institute in Des Plaines, IL, provides basic and advanced courses in safety and health for federal and state compliance officers, state consultants, federal agency personnel, and private sector employers, employees, and their representatives.
OSHA also provides funds to nonprofit organizations, through grants, to conduct workplace training and education in subjects where OSHA believes there is a lack of workplace training. Grants are awarded annually, with a 1-year renewal possible. Grant recipients are expected to contribute 20 percent of the total grant cost.
For more information on grants, training, and education, contact the OSHA Training Institute, Office of Training and Education, 1555 Times Drive, Des Plaines, IL 60018, (708)297-4810.
For further information on any OSHA program, contact your nearest OSHA regional or area office listed at the end of this publication.
STATES WITH APPROVED PLANS
COMMISSIONER
Alaska Department of Labor
1111 West 8th Street
Room 306
Juneau, AK 99801
(907) 465-2700
DIRECTOR
Industrial Commission of Arizona
800 W. Washington
Phoenix, AZ 84007
(602) 542-5795
DIRECTOR
California Department of Industrial Relations
455 Golden Gate Avenue
4th Floor
San Francisco, CA 94102
(415) 703-4590
COMMISSIONER
Connecticut Department of Labor
200 Folly Brook Boulevard
Wethersfield, CT 06 109
(203) 566-5123
DIRECTOR
Hawaii Department of Labor and Industrial Relations
830 Punchbowl Street
Honolulu, HI 96813
(808) 586-8844
COMMISSIONER
Indiana Department of Labor
State Office Building
402 West Washington St.
Room W 195
Indianapolis, IN 46204-2287
(317)232-2378
COMMISSIONER
Iowa Division of Labor Services
1000 E. Grand Avenue
Des Moines, IA 50319
(515)281-3447
SECRETARY
Kentucky Labor Cabinet
1049 U.S. Highway 127 South
Frankfort, KY 40601
(502) 564-3070
COMMISSIONER
Maryland Division of Labor and Industry
Department of Licensing and Regulation
501 St. Paul Place, 2nd Floor
Baltimore, MD 2 1202-2272
(410) 333-4179
DIRECTOR
Michigan Department of Labor
Victor Office Center
201 N. Washington Square
P.O. Box 30015
Lansing, MI 48933
(517) 373-9600
DIRECTOR
Michigan Department of Public Health
3423 North Logan Street
Box 30195
Lansing, MI 48909
(517) 335-8022
COMMISSIONER
Minnesota Department of Labor and Industry
443 Lafayette Road
St. Paul, MN 55155
(612) 296-2342
DIRECTOR
Nevada Department of Industrial Relations
Division of Occupational Safety and Health
Capitol Complex
1370 S. Curry Street
Carson City, NV 89710
(702) 687-3032
SECRETARY
New Mexico Environment Department
Occupational Health and Safety Bureau
1190 St. Francis Drive
P.O. Box 26110
Santa Fe, NM 87502
(505) 827-2850
COMMISSIONER
New York Department of Labor
State Office Building
Campus 12 - Room 457
Albany, NY 12240
(518) 457-2741
COMMISSIONER
North Carolina Department of Labor
4 West Edenton Street
Raleigh, NC 27601
(319) 733-0360
ADMINISTRATOR
Department of Consumer and Business Affairs
Labor and Industries Bldg.
350 Winter St., NE, Room 430
Salem, OR 97310
(503) 378-3272
SECRETARY
Puerto Rico Department of Labor and Human Resources
Prudencio Rivera Martinez Building
505 Munoz Rivera Avenue
Hato Rey, PR 00918
(809) 754-2119
COMMISSIONER
South Carolina Department of Labor
3600 Forest Drive
P.O. Box 11329
Columbia, SC 29211-1329
(803)734-9594
COMMISSIONER
Tennessee Department of Labor
710 James Robertson Parkway
Suite "A" - 2nd Floor
Nashville, TN 37243-0659
(615)741-2582
ADMINISTRATOR
Utah Occupational Safety and Health
P.O. Box 146650
Salt Lake City, UT 84114-6600
(801) 530-6898
COMMISSIONER
Vermont Department of Labor and Industry
120 State Street
Montpelier, VT 05620
(802) 828-2288
COMMISSIONER
Virgin Islands Department of Labor
2131 Hospital Street
Christiansted
St. Croix, VI 00840-4666
(809) 773-1994
COMMISSIONER
Virginia Department of Labor and Industry
Powers-Taylor Building
13 South 13th Street
Richmond, VA 23219
(804) 786-2377
DIRECTOR
Washington Department of Labor and Industries
General Administration Building
P.O. Box 44000
Olympia, WA 98504-4001
(206) 956-4213
ADMINISTRATOR
Occupational Safety and Health Administration
Herschler Building
2nd Floor East
122 West 25th Street
Cheyenne, WY 82002
(307) 777-7672
OSHA CONSULTATION PROJECT DIRECTORY
| State | Telephone |
|---|---|
| Alabama | (205) 348-3033 |
| Alaska | (907) 269-4939 |
| Arizona | (602) 542-5795) |
| Arkansas | (501) 682-4522 |
| California | (415) 703-4441 |
| Colorado | (303) 491-6151 |
| Connecticut | (203) 566-4550 |
| Delaware | (302) 761-8219 |
| District of Columbia | (202) 576-6339 |
| Florida | (904) 488-3044 |
| Georgia | (404) 894-2643 |
| Guam | 011 (671) 475-0136 |
| Hawaii | (808) 586-9100 |
| Idaho | (208) 385-3283 |
| Illinois | (312) 814-2337 |
| Indiana | (317) 232-2688 |
| Iowa | (515) 965-7162 |
| Kansas | (913) 296-7476 |
| Kentucky | (502) 564-6895 |
| Louisiana | (504) 342-9601 |
| Maine | (207) 624-6460 |
| Maryland | (410) 880-4970 |
| Massachusetts | (617) 727-3982 |
| Michigan | (517) 332-1817(H) (517) 322-1809(S) |
| Minnesota | (612) 297-2393 |
| Mississippi | (601) 987-3981 |
| Missouri | (314) 751-3403 |
| Montana | (406) 444-6418 |
| Nebraska | (402) 471-4717 |
| Nevada | (702) 486-5016 |
| New Hampshire | (603) 271-2024 |
| New Jersey | (609) 292-2424 |
| New Mexico | (505) 827-4230 |
| New York | (518) 457-2481 |
| North Carolina | (919) 662-4644 |
| North Dakota | (701) 328-5188 |
| Ohio | (614) 644-2246 |
| Oklahoma | (405) 528-1500 |
| Oregon | (503) 378-3272 |
| Pennsylvania | (412) 357-2561 |
| Puerto Rico | (809) 754-2188 |
| Rhode Island | (401) 277-2438 |
| South Carolina | (803) 896-4300 |
| South Dakota | (605) 688-4101 |
| Tennessee | (615) 741-7036 |
| Texas | (512) 440-3809 |
| Utah | (801) 530-7606 |
| Vermont | (802) 828-2765 |
| Virginia | (804) 786-6359 |
| Virgin Islands | (809) 772-1315 |
| Washington | (206) 956-5443 |
| West Virginia | (304) 558-7890 |
| Wisconsin | (608) 266-8579(H) (608) 266-1818(S) |
| Wyoming | (307) 777-7786 |
OSHA AREA OFFICES
| Area | Telephone |
|---|---|
| Albany, NY | (518) 464-6742 |
| Albuquerque, NM | (505) 248-5302 |
| Allentown, PA | (215) 776-0592 |
| Anchorage, AK | (907) 271-5152 |
| Appleton, WI | (414) 734-4521 |
| Augusta, ME | (207) 916-5783 |
| Austin, TX | (512) 750-3270 |
| Avenel, NJ | (908) 962-2840 |
| Baltimore, MD | (410) 962-2840 |
| Baton Rouge, LA | (504) 389-0474 |
| Bayside, NY | (718) 279-9060 |
| Bellevue, WA | (206) 553-7520 |
| Billings, MT | (406) 247-7494 |
| Birmingham, AL | (205) 731-1534 |
| Bismarck, ND | (701) 250-4521 |
| Boise, ID | (208) 334-1867 |
| Bowmansville, NY | (716) 684-3891 |
| Braintree, MA | (617) 565-6924 |
| Bridgeport, CT | (203) 579-5581 |
| Calumet City, IL | (708) 891-3800 |
| Carson City, NV | (702) 885-6963 |
| Charleston, WV | (304) 347-5937 |
| Cincinnati, OH | (513) 841-4132 |
| Cleveland, OH | (216) 522-3818 |
| Columbia, SC | (803) 765-5904 |
| Columbus, OH | (614) 469-5582 |
| Concord, NH | (603) 225-1629 |
| Corpus Christi, TX | (512) 888-3420 |
| Dallas, TX | (214) 320-2400 |
| Denver, CO | (303) 844-5285 |
| Des Plaines, IL | (847) 803-4800 |
| Des Moines, IA | (515) 284-4794 |
| Englewood, CO | (303) 843-4500 |
| Erie, PA | (814) 833-5758 |
| Fort Lauderdale, FL | (954) 424-0242 |
| Fort Worth, TX | (817) 428-2470 |
| Frankfort, KS | (502) 227-7024 |
| Harrisburg, PA | (717) 782-3902 |
| Hartford, CT | (860) 240-3152 |
| Hasbrouck Heights, NJ | (201) 288-1700 |
| Hato Rey, PR | (787) 277-1560 |
| Honolulu, HI | (808) 541-2685 |
| Houston, TX | (281) 286-0583 |
| Houston, TX | (713) 591-2438 |
| Indianapolis, IN | (317) 226-7290 |
| Jackson, MS | (601) 965-4606 |
| Jacksonville, FL | (904) 232-2895 |
| Kansas City, MO | (816) 426-2756 |
| Lansing, MI | (517) 377-1892 |
| Little Rock, AR | (501) 324-6291 |
| Lubbock, TX | (806) 743-7681 |
| Madison, WI | (608) 264-5388 |
| Marlton, NJ | (609) 757-5181 |
| Methuen, MA | (617) 565-8110 |
| Milwaukee, WI | (414) 297-3315 |
| Minneapolis, MN | (612) 348-1994 |
| Mobile, AL | (205) 441-6131 |
| Nashville, TN | (615) 781-5423 |
| New York, NY | (212) 264-9840 |
| Norfolk, VA | (804) 441-3820 |
| North Aurora, IL | (708) 896-8700 |
| Oklahoma City, OK | (405) 231-5351 |
| Omaha, NE | (402) 221-3182 |
| Parsippany, NJ | (201) 263-1003 |
| Peoria, IL | (309) 671-7033 |
| Philadelphia, PA | (215) 597-4955 |
| Phoenix, AZ | (602) 640-2007 |
| Pittsburgh, PA | (412) 644-2903 |
| Portland, OR | (503) 326-2251 |
| Providence, RI | (401) 528-4669 |
| Raleigh, NC | (919) 856-4770 |
| Salt Lake City, UT | (801) 524-5080 |
| San Francisco, CA | (415) 744-7120 |
| Savannah, GA | (912) 652-4393 |
| Smyrna, GA | (404) 984-8700 |
| Springfield, MA | (413) 785-0123 |
| St. Louis, MO | (314) 425-4249 |
| Syracuse, NY | (315) 451-0808 |
| Tampa, FL | (813) 626-1177 |
| Tarrytown, NY | (914) 682-6151 |
| Toledo, OH | (419) 259-7542 |
| Tucker, GA | (404) 493-6644 |
| Westbury, NY | (516) 334-3344 |
| Wichita, KS | (316) 269-6644 |
| Wilkes-Barre, PA | (717) 826-6538 |
U.S. Department of Labor
OCCUPATIONAL SAFETY AND HEALTH ADMINISTRATION (OSHA)
AND BUREAU OF LABOR STATISTICS (BLS)
REGIONAL OFFICES
Region I
(CT, MA, ME, NH, RI,VT)
OSHA
133 Portland Street
1st Floor
Boston, MA 02 1 14
Telephone: (6 17) 565-7 164
BLS
1 Congress Street
10th Floor
Boston, MA 02114-2023
Telephone: (617)565-2327
Region II
(NJ, NY, PR, VI)
OSHA
201 Varick Street
Room 670
New Your, NY 10014
Telephone: (212) 337-2378
BLS
201 Varick Street
Room 808
New York, NY 10014-4811
Telephone: (212)337-2400
Region III
(DC, DE, MD, PA, VA, WV)
OSHA
Gateway Building, Suite 2100
3535 Market Street
Philadelphia, PA 19104
Telephone: (215)596-1201
BLS
3535 Market Street
P.O. Box 13309
Philadelphia, PA 19101-3309
Telephone: (215)596-1154
Region IV
(AL,FL, GA, KY, MS,NC, SC, TN)
OSHA
1375 Peachtree Street, N.E.
Suite 587
Atlanta, GA 30367
Telephone: (404)347-3573
BLS
1371 Peachtree Suite, N.E.
Atlanta, GA 30367-2302
Telephone: (404)347-4416
Region V
(IL, IN, MI, MN, OH, WI)
OSHA
230 South Dearborn Street
Room 3244
Chicago, IL 60604
Telephone: (312)353-2220
BLS
9th Floor
Federal Office Building
230 South Dearborn Street
Chicago, IL 60604-1595
(312)353-1880
Region VI
(AR, LA, NM, OK, TX)
OSHA
525 Griffin Street
Room 602
Dallas, TX 75202
Telephone: (214)767-6970
BLS
Federal Building
525 Griffin Street
Room 221
Dallas, TX 75202-5028
Telephone: (214)767-6970
Region VII
(IA, KS, MO, NE)
OSHA
911 Walnut Street, Room 406
Kansas City, MO 64106
Telephone: (816)426-5861
BLS
911 Walnut Street, Room 406
Kansas City, MO 64106-2009
Telephone: (816)426-2481
Region VIII
(CO, MT, ND, SD, UT, WY)
OSHA
Federal Building, Room 1576
1961 Stout Street
Denver, CO 80294
Telephone: (303)844-3061
BLS
911 Walnut Street
Kansas City, MO 64106-2009
Telephone: (816)426-2481
Region IX
(American Samoa, AZ, CA, Guam, HI, NV, Trust Territories of the Pacific)
OSHA
71 Stevenson Street
Room 420
San Francisco, CA 94105
Telephone: (415)744-6670
BLS
71 Stevenson Street
P.O. Box 193766
San Francisco, CA 94119-3766
Telephone: (415)744-6600
Region X
(AK, ID, OR, WA)
OSHA
1111 Third Avenue
Suite 715
Seattle, WA 98101-3212
Telephone: (206)553-5930
BLS
71 Stevenson Street
P.O. Box 193766
San Francisco, CA 94119-3766
Telephone: (415) 744-6600
These states and territories operate their own OSHA-approved job safety and health programs (Connecticut and New York plans cover public employees only). States with approved programs must have a standard that is identical to, or at least as effective as, the federal standard.

